|
MYCOBACTERIAL
SKIN INFECTIONS
|
|
|
|
Tuberculosis in the newborn due to transmission of infection in utero is relatively rare. The mother‘s genital tract is probably often the source of the infection . Classification of skin tuberculosis Tuberculosis of the skin has different clinical and pathological features depending on the patient‘s resistance and age .
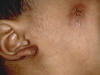
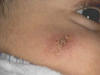
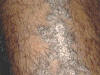
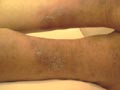
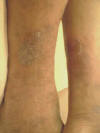
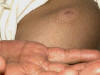
This is the most common and most variable type of cutaneous tuberculosis. This is a destructive form of TB of the skin affecting mainly the exposed areas of skin on the face and extremities.
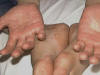
Fig. 50a. Lupus Vulgaris Fig. 50b. Lupus Vulgaris Fig. 50ac. Lupus Vulgaris
CLINICAL MANIFESTATIONS The primary skin lesions appear as reddish brown plaques, which have a chronic course and heal slowly in one area and progress peripherally in another. The ulcers heal with scar tissue leading to destruction and configuration. The nodules have an apple-jelly color and on diascopy show the distinctive apple-jelly yellowish brown color. Histopathology The histopathology of lupus vulgaris is characterized by:
PRIMARY
TUBERCULOUS COMPLEX Primary complex lesions involve the skin and lymph nodes mainly that of infants and young children . The route of entry of tubercle bacilli is the lung. The common sites involved are the face and extremities associated with regional lymphadenopathy. CLINICAL FEATURES The most common sites involved are the face and extremities. Mucous membrane are involved in about one third of cases. The lesion appears as brownish red papule that becomes later on an indurated nodule or plaque. These lesions take few months to heal while the enlarged lymph glands persist longer and ulcerate . Histopathology Marked inflammatory response with many Polymorphonuclear leukocytes and tubercle bacilli in the first two weeks. Lymphocytes and epitheloid cells appear later and replace the polymorphs.
This type occurs usually in infants and young children. Dissemination of the disease occurs, often following measles and scarlet fever or other exanthomas. CLINICAL FEATURES Skin manifestations are often variable. The lesions may appear as generalized acute eruption of brownish red accuminate papules that may ulcerate forming numerous minute ulcers. These ulcers are necrotic , small , circular and covered by seropurulent exudate.
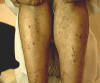
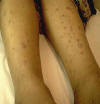
This type of lesion occurs mainly in young children and adults who have TB elsewhere in the body. This is considered as an allergic reaction to tubercle bacilli.Tuberculids are probably due to the hematogenous dissemination of tubercle bacilli in a person with a moderate or high degree of immunity, but the underlying focus of tuberculosis may not be clinically active at the time of the eruption, and the patient is often in excellent health. CLINICAL FEATURES The lesions appear as small firm follicular brownish pinhead papules that occur symmetrically on the limbs, mainly on the extensor surface, trunk and face.
Fig.51c. Papulonecrotic tuberculid (Fresh lesion) Central necrosis of the lesions may follow, ending with small-pitted scars. The lesion occurs over the trunk mainly in children having tuberculosis of the bone or lymph nodes. Skin presents with firm, flat-topped hyperkeratotic papules surmounted by pustule or tiny scales, arranged in groups and have a very chronic course. The lesions may undergo spontaneous involution and may recur again.
This type occurs mainly in adults and in individuals with high resistance due to external inoculation of tubercle bacilli. CLINICAL FEATURES The lesion appears mainly on the extremities, on the dorsum of the fingers, hands, ankles and buttocks as single hyper keratotic red dull lesion. This is characterized by a very chronic course that may be accompanied by lymphangitis, lymphadenitis and rarely by skin gangrene.
Fig.31d. Tuberculosis verrucosus cutis DIFFERENTIAL DIAGNOSIS
ERYTHEMA
INDURATUM Erythema induratum is a chronic benign vasculitis of the subcutaneous arteries and veins accompanied by fat necrosis. Erythema induratum has been included as a manifestation of tuberculosis of skin, which can be caused, by Mycobacterium tuberculosis until recently where it is considered a type of vasculitis. This was supported by the clinical response and the healing of lesions by corticosteroids rather than by antituberculous medications.
CLINICAL FEATURES Soft recurrent indolent subcutaneous nodules symmetrically distributed on both legs , mainly in young females . The lesions tend to heal within few months and recur again. The covering skin becomes later dusky or bluish in color with soft center that later may show irregular excavated ulceration. The lesions are mildly tender.
Scrofuloderma occurs mainly in children and young adults on the skin over the cervical lymph nodes or above the bony areas. The lesion develops secondarily to the underlying infected lymph nodes which break down and cause stretch of the superimposed skin leading to ulceration and sinus formation. CLINICAL FEATURES The skin covering the inflamed lymph nodes becomes indurated , purplish in color followed by ulceration with crusty ,irregular pale granulomatous tissue ending in scarring.
TUBERCULOSIS CUTIS ORIFICIALIS Young adults and children with complete anergy are affected by this type, which is usually accompanied by visceral TB. The lesions involve the mucous membranes of the mouth, palate, larynx, intestinal and lung mucous membranes. CLINICAL FEATURES The lesions begin with an oval shallow crusted ulcers extending to the adjacent areas, which run a very chronic course. DIAGNOSIS Several data may suggest the diagnosis of cutaneous tuberculosis mainly:
TREATMENT OF CUTANEOUS TUBERCULOSIS Different courses are used for treatment of tuberculosis.More than antituberculous drug is given to prevent bacterial resistence.The course of treatment is a long one that may take several months.
These drugs should be given together.Another anti-tuberculous drug is usually given in combination of these drugs. Another regimen(adult doses) for treatment of tuberculosis is : Isoniazid 3oomg, Rifampicines 600mg, Pyrazinamide 2gm and streptomycin 1gm or Ethambutol 15mg/kgm qd for 2 months followed by one of the following: Isoniazid 300mg and rifampin 600mg qd for 4 months or Isoniazid 900mg,rifampin 600mg qd for 4 months. Para-amino salicylic acid(PAS): is used only as concomitant therapy with INH or streptomycin. Vaccination: a vaccine containing polysaccharide prepared from a pure human-type tubercle bacilli was tried for treatment of cutaneous tuberculosis with encouraging results. All drugs are taken on an empty stomach once daily.
BCG VACCINATION Currently used strains, maintained BCG (bacille Calmette-Guerin) vaccines owe their origin to the in vitro attenuation by Calmette and Guerin. Vaccination protects the host by blocking the secondary hematogenous spread of the pathogen, limiting the primary infection to subclinical proportions. The protective effect of BCG in children is likely to last at least 15 years. High-risk groups, such as hospital workers or travellers to areas of high prevalence are advised for vaccination . Fig. 35c.&d Exfoliative dermatitis after B.C.G vaccination The technique of vaccination should be as follows : The vaccine should be reconstituted fresh for each session and given by intradermal injection into the skin of the left upper arm in the sulcus over the insertion of the left deltoid muscle. A separate 1ml plastic syringe and short bevel gauge 25 needle should be used for each patient . The dose for infants is 0.05 ml , older children and adults are given double of this dose . A local reaction usually occurs 2 to 6 weeks after vaccination as a small papule that may slowly enlarge and discharges purulent material to leave a shallow ulcer.
|
| Contents | << Previous Chapter | Next Chapter >> | Search |