|
The cutaneous
manifestations of congenial syphilis tend to appear during the first few
weeks or months of life. Syphilis is transmitted from the mother to the
fetus via the placenta. The infection is therefore prenatal rather than
congenital.
Skin
manifestations of early congenital syphilis
-
Stigmata
Congenital syphilis
can be easily diagnosed in the presence of stigmata. Stigmata are
found in young children due to destructive lesions of syphilis leading
to scarring.
These changes are
known as " Hutchinson‘s triad" which include:
-
Saddle nose
-
Skin rhagades (radial
scars)
-
Corneal ulcers and
opacities
-
Hutchinson‘s teeth
and mulberry moles.
-
Syphlitic
PemphigusSymmetrical bullous eruption may be found on the palms and
soles. Seropurulent fluid laden with treponemas comes out from the
lesion. Later on crust covers the dull red eroded area.
-
Condyloma Lata
These lesions may
affect muco- cutaneous junction.
Clinical
features
Mucous
membranes manifestations
Ulceration and
destruction of the mucous membranes occur in the infected areas .
The mucous membrane of
the nose mouth, throat and larynx are affected where muco-purulent
discharge or blood stained discharge exudes from the nose. This is called
"snuffles."
The infant has an aphonic
cry due to involvement of the larynx.
Skin
manifestations
The skin becomes red,
glazed and radiating fissures may appear at the angles of the mouth,
around the nares and anus. Healing of these lesions lead to formation of
radial scars known as "rhagades"
Systemic
Manifestations
-
Old man look - due to
constitutional symptoms as gastro-enteritis, pneumonia, weight loss
and marasmus, which lead to wrinkled yellow brown skin.
-
Syphilitic alopecia
-
Scalp - the sides and
back of the head show areas of hair loss, has the characteristic of
"moth eaten" appearance.
-
Eye lashes and
eyebrows are absent.
-
Nail dystrophy.
SKIN
MANIFESTATIONS OF LATE CONGENITAL SYPHILIS
Late congenital syphilis
causes a wide variety of signs and symptoms in untreated cases. A benign
tertiary lesion is rare under the age of 5 years. A number of these are so
characteristic:
-
Gumma :Gummatous
ulceration of the mouth and nose where there may be perforation of the
nasal septum with deformities of the nose.
Destruction to the
palate may cause regurgitation of food.
-
Stigmata : due
to scarring from the early lesions.
Saddle nose
Rhagades around the
mouth, nostril and anus.
Diagnosis
of congenital syphilis
By the clinical picture.
Serological tests: VDRL
,TPI and FTA-ABS (IgM).
TREATMENT
OF CONGENITAL SYPHILIS
It is very important to
diagnose and treat the mother and contacts, as siblings. Contact -tracing
should be considered.
Penicillin injection is
the drug of choice.
Recommended dose for
infants and children: Procaine penicillin 450,000 unit per kg body weight
for 10 days.
Benzathine penicillin:
may be administered for congenital syphilis as a single intramuscular
injection of 50,000 units per kg. body weight .
Erythrocin can be given
for 2-3 weeks when there is sensitivity to penicillin.
NON
VENEREAL TREPONAEMAS
YAWS
Yaws is a non-venereal
systemic infectious disease that begins frequently in childhood. The
course of the disease in children is more rapid than in adults.
Treponema pertenue is the
causative organism that is endemic in certain tropical areas.
Etiology
The causative organism
Treponema pertenue is identical morphologically with T. palladium of
syphilis. Flies of the genus Hippelates transmit infections to human
beings. Mild trauma and even skin abrasion may facilitate seeding of the
organisms into the skin.
Clinical
features
-
The
early stage
Primary lesions -
primary papule or groups of papules appear within one month or more after
the organism enters the skin. This primary lesion is called
"frambesiform" and localized to the skin only without
involvement of internal organs. Infection is non-venereal and is not
transmitted congenitally.
-
Secondary lesions
- these lesions appear as amber-yellow, soft, crusted frambesiform
granulomatous nodules on the face and extremities. The lesions usually
heal without destruction or scarring. The lesions heal with mild
atrophy and some depigmentation where later these lesions become hyper
pigmented. Pigmentation is severe in palmer and plantar lesions. They
may not be easily diagnosed clinically and may resemble some common
skin diseases.
-
Tertiary stage:
this stage may appear after a long chronic course extending years
after the primary stage where there is numerous relapses and
spontaneous cure may occur.
-
Late tertiary
stage of yaws - may end with horrible destruction of the skin and
bones leading to disfiguration.
Manifestations of late
tertiary stage:
Systemic manifestations
are more severe in children. These include low-grade fever, malaise, and
generalized lymphadenopathy.
Some disability may
result from involvement of palms and soles. Periosteitis and rarefaction
are more extreme in children.
Skin lesions are large
nodules that may reach up to 15 cm. in diameter with ulceration where
healing occurs in certain areas, and new lesion extending to a new area
causing more destruction. The scarring leads to atrophic and
hyperpigmented areas.
Lesions of the palms and
soles show extensive thickening and superficial ulcerations with
vegetative annular lesions.
Absence of mucous
membrane lesion in the secondary stage differentiates yaws from syphilis.
Absence of congenital
transmission in yaws.
Involvements of internal
organs are very rare in late tertiary stage of yaws.
Diagnosis
-
Typical clinical
picture.
-
The presence of
characteristic lesions of the palm and soles in an endemic area is
diagnostic.
-
Demonstration of the
spirochetes by dark field.
-
Positive serological
test for syphilis.
Treatment
Penicillin is the
drug of choice.
WHO recommended dosage
for treatment of Yaws is as follows:
-
Procaine penicillin
in oil with aluminium monostearate (PMA ) as a single dose for
children under 15 years old is 600,000 units .
-
Patients above 15
years old needs 1,200,000 unit for active cases of yaws
-
Latent cases and
contacts need half the dose of children under 15 years old. (300,000
units)
PINTA
Pinta is a non-venereal
treponemal infection called "blue stain disease."
Peculiar pigmented
patches of the skin, affecting mainly colored races characterize the
disease. It is caused by Treponema carateum that is indistinguishable
morphologically from the organisms causing syphilis and yaws.
The disease is endemic in
tropical and subtropical regions.
Modes
of Infection
-
Flies of the genus
Hippelates transmit the infection.
-
Direct contact with
the patients.
-
During the first
stage, infected babies may infect their mothers during breast-feeding
by direct contact where a breast chancre may develop.
Clinical
Picture
The incubation period is
similar to other treponemal infections
|
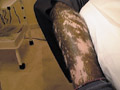
Fig. 55. Pinta |
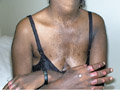
Fig. 56a. Pinta
|
-
Primary
stage
This stage begins
after one to several weeks from infection .
The lesions begin
as a tiny red papule on the legs and on the exposed areas that
becomes elevated ill-defined erythematous plaque.
Satellite papules
may surround the primary lesion after few months and fuse together
forming configuring patterns.
No ulceration
of the lesion and that characterizes Pinta from syphilis.
STS are non-reactive
in the primary stage and dark field examination may be positive.
-
Secondary
stage
This stage will
take from 5-12 months to appear following the primary stage.
The lesions may be inconspicuous and may pass without notice.
|
The lesions appear as
erythematous circinate patches mainly on the extremities and to lesser
extent on the face.
STS is reactive in 60
percent in the secondary stage. Spirochetes may appear in aspirated lymph. |
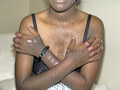
Fig. 56b. Pinta
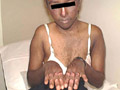
Fig. 57. Pinta (Blue stain disease)
|
-
Late
stage
This stage appears after
a very long course taking years in adults and has a very chronic course.
The lesions appear on the face, head and neck as stippled discrete or
localized slate blue pigmentation and replaced after a long time by
depigmented spots resembling vitilligo. Hence this stage is sometimes
called "dyschromic stage". The skin shows blue patches (blue
pinta) and white areas (white pinta ) . The lesions may become
hyperkeratotic.
Skin gummata may end in
deep ulceration and destruction of the sites involved in the skin, bones
and nose, and rarely the pharynx leading to extensive deformities.
Involvement of the
internal organs and neurological manifestations are rare .
Treatment
Penicillin is the
drug of choice .
The recommend dose for
adults is four injections of Benzathine penicillin 1,200,000 units every
four days. The blue color, the depigmented areas and the hyperkeratotic
lesions begin to disappear after treatment.
BEJEL
Bejel is an endemic non
venereal disease. Large percentage of the population in the endemic areas
is infected before puberty. Their children may infect adults who escape
infection in childhood . There is no evidence of transmission in utero.
|
CLINICAL
MANIFESTATIONS
Primary stage:
primary lesion usually is not apparent and the manifestations present with
the secondary stage.
|
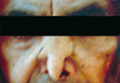
Fig. 58. Bejel
|
Secondary stage:
manifests with generalized papular , annular papular and papulo-squamous
eruption . Mucous membrane involvement is in the form of condylomas and
mucous patches which simulate other manifestations of endemic Treponema .
Hoarseness of the voice and nocturnal bone pains are common and
characteristic symptoms .
Latent stage :
this stage manifests, with destruction of bone, tissues, systemic
involvement of cardiovascular and nervous system .
Treatment
The same as other types
of non-venereal treponemas.
REFERENCES
-
Boot JM, Oranje AP,
Menke HE et al. congenital syphilis in the Netherlands: diagnosis &
clinical features. Genitourin Med 1989; 65: 300-3.
-
Bradlaw RV. The dental
stigmata of prenatal syphilis. Oral Surg Oral Med Oral Pathol 1953; 6:
147-58.
-
Browne SG. Yaws. Int J
Dermatol 1982; 21: 220-3.
-
Bengali FS. Involvement
of aortic valve and ascending aorta in congenital syphilis. Br J Vener
Dis 1961; 37: 257-67.
-
Dunlop EMC, Wink RB.
Incidence of corneal changes in congenital syphilis. Br J Vener Dis
1954; 30: 201-9.
-
Feign D, Glenn M,
MacBride-Stewart G et al. Yaws in the Solomon Islands. J Trop Med Hyg
1990; 93: 52-7.
-
Harter CA, Benirschke
K. Fetal syphilis in the first trimester. Am J Obstet Gynecol 1976; 124:
705-11.
-
Hackett CJ, Loewenthal
LJA. Differential Diagnosis of Yaws. Monograph Series, No. 45. Geneva:
WHO, 1960.
-
Mascola L, Pelosi R,
Blount JH et al. Congenital syphilis revisited. Am J Dis Child 1985;
139: 57-80.
-
Medina R. Pinta. An
Endemic Treponematosis in the Americas. WHO INT/VDT/204.65.
-
Noordhoek GT, Cockayne
A, Schouls LM et al. A new attempt to distinguish serologically the
subspecies of Treponema pallidum causing syphilis and Yaws.J Clin
Microbiol 1990; 28: 1600-7.
-
Robinson RCV.
Congenital syphilis. Arch Dermatol 1969; 99: 599-610.
-
Willcox RR. Njovera: an
endemic syphilis of Southern Rhodesia. Lancet 1951; i: 558-60.
-
Whittet HB, Quiney RE.
Nasal manifestation of yaws. J Laryngol Otol 1988; 102: 1147-9.
-
Hackett CJ, Loewenthal
LJA. Differential Diagnosis of Yaws. MonographSeries, No. 45. Geneva:
WHO, 1960.
-
Mascola L, Pelosi R,
Blount JH et al. congenital syphilis revisited. Am J Dis Child 1985;
139: 57-80.
-
Noordhoek GT, Cockayne
A, Schouls LM et al. A new attempt to distinguish serologically the
subspecies of Treponema pallidum causing syphilis and Yaws.
-
WHO. Treponemal
infections. Technical Report Series No. 674. Geneva: WHO,1982.
-
WHO. Expert Committee
on Venereal Diseases and Treponematoses. Sixth Report. Technical Reports
Series No. 736. Geneva: WHO, 1986.
TROPICAL ULCER
Tropical ulcers occur in
the tropical areas during the rainy seasons. The disease is more common in
school children .
Different organisms such
as pyogenic organisms, syphilis , yaws and Vincent‘s angina may cause
tropical ulcer.
CLINICAL
FEATURES
The lesion begins as an
inflammatory papule, frequently on a pre-existing abrasion or mild trauma
on the legs and arms. The lesion is usually single and unilateral,
meanwhile it is not uncommon to find multiple ulcers upon both legs. The
papule is transformed into a vesicle, which ruptures leading to an ulcer. The
ulcer may be small or large with elevated or depressed smooth, ragged and
undermined edges.
|
Differential Diagnosis:
Different ulcers should
be differentiated from tropical ulcer.
Diphtheria ulcer:
the
ulcer is small, superficial and mycobacterium diphtheria can be isolated.
Tuberculus ulcer:
the
ulcer is undermined, rarely on the leg and tubercle bacilli can be
detected in the skin lesion. |
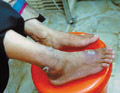
Fig. 59a. Tropical ulcer
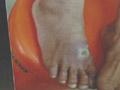
Fig.59b.Tropical
ulcer
|
|
Syphilitic
ulcer: the ulcer is punched out with sinking floor. Serological tests
for syphilis are positive.
Leprosy: can be easily
diagnosed due to neurological manifestations and its late manifestations
that are diagnostic.
Leishmania ulcer: the
course of the ulcer is very chronic in an endemic area and the organism
can be isolated from the lesion.
Varicose ulcer: irregular
and shallow, the edges are covered by thin, blue line of growing
epithelium, while the base consists of pink, granulation tissue and
located on the lower part of the shin which shows also dilated veins.
Mycotic ulcer:
superficial, nodulo ulcerative and the causative fungi can be easily
isolated from the lesion.
Frambesia ulcer: occurs
in endemic areas, has rapid course and Treponema pertenue can be detected.
Treatment
-
Preventive measures
are very important against insect bites and other predisposing factors.
-
Systemic and topical
antibiotic.
-
Treatment of the
causative organism.
VERRUGA
PERUANA
(Carrion‘s Disease)
This is an infectious
constitutional disease caused by Bartonella bacilliforms that may affect
young ages and infants where a long lasting immunity develops . The
disease is endemic in certain valleys in central part of south America
occurring mainly in the rainy season. The sand fly vectors are the
Phlebotomus noguchi and P. verrucarum which transmit the disease.
CLINICAL MANIFESTATIONS
The clinical
manifestations present in two forms :
-
Mild form is
accompanied by characteristic skin manifestations.
-
General
Manifestations: vague Prodromal symptoms manifest with simple anemia.
-
Skin manifestations:
The skin rash has
symmetrical distribution , which is of two types :
The miliary type: which
is in the form of pinhead to pea size, cherry red, hard discrete, sessile
or pseudo pedunculated lesions, appearing on the face and extremities.
The nodular type: Deep
nodules begin in the subcutaneous tissue over the elbows and subcutaneous
tissue.
The more profuse the
eruption the better is the prognosis .
-
The severe type
(Oroya): The only skin manifestations are mild skin lesion due to insect
bite at the site of inoculation .
This type is acute
followed by a chronic course presenting with verrucous skin lesions.
Systemic manifestations:
-
Fever and malaise .
-
Anemia, which may be
severe .
-
Leukopenia .
-
Later cherry red ,
hard multiple verrucous lesions develop one to two months after recovery
from the febrile stage .
Treatment
| 1. Prophylaxis |
2.
Penicillin |
3. Systemic corticosteroids.
|
REFERENCES
-
Adriaans B, Hay RJ,
Drasar B et al. The infectious aetiology of tropical ulcer - a study of
the role of anaerobic bacteria. Br J Dermatol 1987; 1616: 31-7.
-
Robinson DC, Adriaans
B, Hay RJ et al. The epidemiology and clinical features of tropical ulcer.
Int J Dermatol 1988; 27: 49-53.
-
J Clin Microbiol 1990;
28: 1600-7 .
-
Wilkinson M, Agett P,
Cole TJ. Zinc and acute tropical ulcers in Gambian children and
adolescents. Am J Clin Nutr 1985; 41: 43-51.
|
Top
|






