|
NEONATAL CONTACT DERMATITIS
|
|
|
|
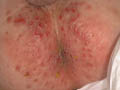
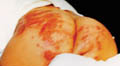
Diapers: especially with plastic coatings has more irritating effect when left unchanged for a long period due to direct irritating effect or by the secretions of urine , feces and ammonia, which may cause contact eczema . Metals :Earrings or other metals may initiate a local eczematization . Perfumes or perfumed tissue paper has also an effect . Wool and polyester in the dressings , covers or rags , carpets and blankets are common cause of contact dermatitis . Cosmetic preparations : Such as cream, ointment and lotions. Talcum powders or antiseptics containing hexa chlorophene is not only irritant but may cause hazardous toxic effects. Medicated creams containing antibiotics such as neomycin, sulfa, penicillin, antihistamines and even corticosteroids may cause contact dermatitis but mainly of the delayed type hypersensitivity. This may be due to the active ingredients or due to the base or the added materials . Clinical Features Contact dermatitis in the newborn is usually acute, where there may be an erythematous, oozing , vesicular or bullous lesions at the site of contact. The condition may become chronic if neglected leaving an erythematous dry scaly patches . Itching in the newborn is expressed by different ways; either in the form of irritable newborn moving from one side to another or to rub the area towards his mother during breast feeding or fondling . Patch testing is sometimes of help to spot the irritating agent in older infants and children . Treatment Elimination and stop contact with the sensitizing agent comprises the most important factor in the management of irritant dermatitis . Pufexamac creams (Parfenac or Droxaryl) is usually enough to control mild cases . Severe cases may require mild hydrocortisone topically . Antihistamine may be used to relieve itching.
Intertrigo is a term applied to an inflammatory reaction, which is more or less confined to the major body folds. Intertrigo may be an eczematous reaction or inflammation of the intertriginous areas due to bacterial or fungal infections. Bacterial and fungal intertrigo was discussed in the previous chapters .
It should be noted that infants and children may be exposed directly to the different allergens or to those available in the house or around or allergens used by the mother such as cosmetics for hair, nail, creams, perfumes or many others. Different substances may act as allergens in infants and young children. Some of these include the fillowing: The widespread use of toxic applications such as antiseptics . Prolonged skin contact with urine and feces . The frequent presence of occlusive conditions by diapers and others Most eczematous reaction in infants is transient manifesting only with mild symptoms while others may be severe . Predisposing Factors: Different predisposing factors may lead to eczematous intertrigo. Combination of moisture and friction in opposing skin surfaces. Obesity is a common predisposing factor. Over warming of the crural area by clothing or due to hot humid , damp weather. Poor hygiene . Occlusion of the crural areas . External irritants : different irritants may predispose to eczematization of the body folds . Some of these include the following : Detergents, antiseptics, topical medications, cosmetics as perfumes , deodorants, and excessive powders especially those containing small crystals not finely powdered or containing irritant or toxic substances . Clinical Features Skin lesions present with sharply marginated erythema on the crural areas mainly on the side of thighs, axilla and anal cleft. The margins remain sharp but often may develop a characteristically scalloped outline. Pustules often develop within and just beyond the periphery. The condition may become extensive spreading peripherally to the adjacent tissue. Maceration and chaffing especially in well nourished obese infants and children leads to secondary bacterial and fungal infections . Continuous occlusion of the areas may lead to miliaria due to obstruction of the sweat duct orifices . Secondary bacterial and fungal infection, particularly Candida albicans is common especially in infants using diapers. In severe cases the affected areas become eroded showing pustules or even abscesses . Diagnosis The clinical features of intertrigo overlap with those of primary irritant napkin dermatitis, "seborrheic" dermatitis of infancy, atopic dermatitis and psoriasis. The diagnostic separation of these disorders is not always possible meanwhile, initial treatment is so similar. Treatment of Intertrigo Treatment is essentially the same as that for primary irritant napkin dermatitis and infantile atopic dermatitis Since secondary infection appears to be common, antibiotics alone or combined with anti-candida preparations may be used. Differential Diagnosis
Treatment Mild cases: Drying of the crural area by application of an appropriate mild antimicrobial dusting powder such as Zeasorb. Talc should be avoided as it is abrasive and likely to aggravate the eruption. I usually use non-steroid anti-inflammatory topical preparation alone such as Pufexamac (Droxaryl) or in combination with anti-bacterial and antifungal preparation such as (Flogocid, Parfenac cream )These are safe and effective. In more severe cases: the use of mild topical corticosteroids, in combination with anticandida or antibacterial agents (Decoderm compound cream), is indicated, together with frequent applications of an oily emollient to reduce friction. Where the affected area is eroded and weeping, initial treatment with wet compresses containing weak solutions of potassium permanganate 1: 9000 or aluminium acetate may be very helpful. Careful attention should be paid to correct the predisposing factors such as aeration of the crural areas and obesity. Intermediate gauze such as Vaseline gauze or Sofratulle gauze can be applied on the crural areas separating the crural parts from direct contact with diapers in infants has an important role in preventing irritation. The gauze can be used after applying the topical preparation to the intertrigenous areas.
PERI-ANAL DERMATITIS OF THE NEWBORN Etiology Perianal dermatitis has been reported to be more in bottle fed infants due to the higher pH of cow‘s milk. Clinical Features Usually the skin lesions appear early, where the severity of the rash depends on different factors mainly the general condition of the infant, susceptibility to the allergen, repeated exposure and general cleanliness. Mild cases The skin lesion is localized around the perianal area presenting with erythema. Severe lesions: the affected skin may be edematous and superficially eroded. The lesion may extend to other areas such as the crural area leading to napkin dermatitis. General cleanliness . The mother personally should take more care to her child and not leave that to housemaids or nurseries . Changing the diapers whenever wet . Avoidance of strong detergents and soaps for cleaning the area . Avoid irritants as chaffing, occlusion of the skin, alcohol swabs, Dettol and others. Specific Treatment Mild cases may need no treatment . The affected area should be washed as soon as possible after defecation with water and applying water-miscible emollient. White soft paraffin or olive oil applied afterwards can help as a protective lubricant. Moderate cases need non-steroid anti-inflammatory topical preparation such as Pufexamac. Antibiotics or anti fungal preparations may be needed according to the condition . Severe cases may need topical hydrocortisone alone or in combination with antifungal or antibacterial preparations when there is secondary fungal or bacterial infection
This term has been applied to a condition, which arises as a complication of the primary irritant type of napkin dermatitis mainly due to the use of plastic pants or due to topical preparations. Candida albicans has also been considered as an important etiological factor . Clinical Features The skin lesions appear between the fourth and ninth months of life. The lesions comprise one or several rather uniform, livid purple nodules, which are usually oval in outline with their long axis parallel to the skin creases . They persist for some weeks and may leave atrophic scars after healing.
|
| Contents | << Previous Chapter | Next Chapter >> | Search |