|
An adverse
drug reaction may be defined as undesirable clinical manifestations,
consequent to, and caused by administration of a particular drug.
Drug
reactions may be non immunologic or immunologic .
-
Non-immunologic Drug Reactions
Non-immunological
reactions are related to different factors mainly:
Overdose:
leads to different side effects depending on the specific drug.
Certain drugs are hepatotoxic as phenothiazine derivatives and
erythromycin osteolate.
Bone marrow
depressant drugs, certain types of antihistamines, grisoefulvin,
sulphapyridine, sulphones and chloromycetin.
Aspirin,
anti-malarial drugs, sulphones may cause hemolysis.
Cumulative :
certain drugs may have cumulative side effects . Other drugs may
cause different reactions such as the yellowish skin discoloration
due to Atabrine intake or the slate gray color due to silver
compound intake. Hypervitaminosis A may lead to periosteal swelling
in children and hair fall.
-
Immunologic Drug Reaction
Drug
reactions may arise as a result of immunological drug allergy.
This type of
drug reaction is the most common. Drugs may induce different skin
reactions simulating most various skin diseases. Immanologic drug
reaction may present with different skin manifestations. Some of
these are:
Urticaria:
Some of the drugs inducing urticaria are Aspirin, Penicillin.
Eczema:
Topical sensitizers as local anesthetic, topical antihistamines,
topical antibiotics as neomycin, penicillin, halogenated
salicylanilides.
Oral
sensitizer: Sulfonamides, Naldixic acids, and Chloropromazine.
Epoxy
acrylates in filling materials often also react to epoxy resin
leading to local sensitization of the oral mucosa.
Serum
sickness: Penicillin
Exfoliative
dermatitis: Topical sensitizer, heavy metals, and antibiotics.
Fixed drug
eruption: Sulfonamides, barbiturates, and phenolphthalein.
Exanthemata
reaction: Antibiotics, phenylbutazone, thiazides, and barbiturates.
Erythema
multiform: Sulfonamides and others
Epidermal
necrosis: Barbiturates, phenylbutazone and sulfonamides.
Purpura:
Penicillin and cytotoxic drugs.
Granuloma:
Zirconium topically in antiperspirant and cosmetics used topically
especially to the axillary folds, bromides, and iodides.
Lupus
erythematosus -like reaction: Hydrallazine, procainamide.
Hyperpigmentation:
ACTH, Chloropromazine, Busulphan, metals locally as silver nitrates
in topical medications such as that used topically for treatment of
burns.
Hirsutism:
androgens, corticosteroids, and testosterone.
Alopecia:
Cytotoxic drugs, heparin, corticosteroid.
Phototoxic
reaction: due to antimalarial drugs, coumarin and phenothiazines.
The
commonest drugs that may cause skin reactions are:
Antimicrobial
agents:Topical or systemic antibiotics may cause sensitization.
The most
common topical anti-microbial preparations causing allergic contact
dermatitis are: Neomycin, Framycetin, Virginiamycin, and Bacitricin.
Chloro- and
bromosalicylanilides, organic mercury compounds benzyl alcohol,
xanthocillin, sulphonamides, thiuram sulfides, iodine, and bithionol
in shampoos may cause also drug reaction. Systemic antibiotics such
as.
Minocycline,
Chloramphenicol, Penicillin and Tetracyclines may cause different
clinical types of skin reactions.
Ampicillin
and its derivatives may elicit morbilliform rash. The eruption
appears on the
extremities that may become generalized. The onset may be immediate
, occuring in patients treated
with Ampicillin . Usually skin rash develops after one week from the onset
of therapy. Re-exposure of such patients to Ampicillin and other
penicillin derivatives is contra-indicated.Ampicillin in such cases may cause
anaphylactic reaction .
Amoxicillin
:leads to cutaneous eruptions including urticaria, morbilliform, or
maculopapular rashes , fixed drug eruption and serum sickness.
Hydroxyquinolines:
Sterosan and Vioform (Chinoform), as well as esters of
hydroxybenzoic acids (Nipagins, Parabens) Chloroacetamide and
Chloroxylenol have sensitizing capacity. Less common sensitizers are
quaternary ammonium salts in eardrops and antiperspirants.
Antimycotic
agents
Most of the
organic compounds used as antimycotics have sensitizing properties,
e.g. hydroxyquinolines, esters of hydroxybenzoic acid, Jadit
(photosensitizer), thiuram sulfides, organic mercury compounds,
dichlorophene, tolnaftate, nystatin and various other halogenated
phenols compounds (photosensitizers).
Antiviral
agents
Acyclovir ,
amantadine , tromantadine and idoxuridine can all cause
sensitization .
Antihistamines
The
Phenothiazines are the strongest sensitizers, but all can cause
sensitization when used topically .
Corticosteroids
Sensitization
is more common than previously thought. Dermatologists and
physicians are often faced with common steroid side effects due to
abuse or misuse of steroids.
Patients
feel relief of their skin problem and therefore continue using this
double-wedged medication for longer periods leading later to
unwanted side effects .
Local
anesthetics
Derivatives
of P-aminobenzoic acid such as benzocaine, amethocaine, procaine and
dibucaine are strong sensitizers. Mepivacaine (carbocaine) and
lidocaine (lignocaine, Xylocaine) seem to be rare sensitizers.
Non-steroid
anti-inflammatory drugs
The
propionic acid derivatives, such as ketoprofen, ibuprofen, ibuproxam
and tiaprofenic acids, cause contact and photocontact dermatitis,
with cross-reactivity. Topical benzydamine is also a contact and
photocontact sensitizer.
Vitamins
Vitamins A,
E and K, and dexpanthenol have all a sensitizing effect in topical
medicaments in susceptible individuals .
Quaternary
ammonium compounds
They are
used as disinfectants.Quaternary ammonium compounds may cause
sensitization .
Dequalinium
and Cetrimide have produced unusual necrotic lesions in some
individuals, especially when used concentrated and under occlusion.
Ointment and
cream bases
Lanolin,
cetyl, oleyl and stearyl alcohol, ethylene, hexylene and parabens
propylene glycol, linnet wax, white and yellow petrolatum, sesame
and olive oils, perfume, polidocanol and preservatives are known to
be sensitizers. Ethylenediamine can cause also skin sensitization .
|
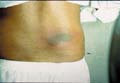
Fig. 238. Fixed Drug Reaction (Sulfonamides)
|
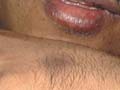
Fig. 239. Fixed drug reaction (Phenothiazine)
|
|
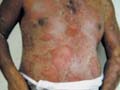
Fig. 240.Drug Reaction
(Amoxicillin Exfoliative dermatitis)
|
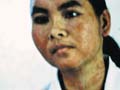
Fig. 241.Drug Reaction (Corticosteroids)
|
|

Fig. 242. Drug Reaction
(Doxycycline)
|
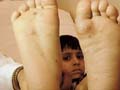
Fig. 243. Bllous Drug Reaction
|
|
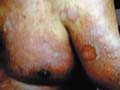
Fig. 244. Drug Reaction
(Exfoliative dermatitis)
|
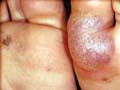
Fig. 245. Bllous Drug Reaction
|
|
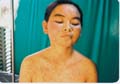
Fig. 246.Drug Reaction (Corticosteroid)
|
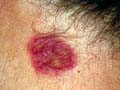
Fig. 247. Fixed Drug Reaction
(Brufen)
|
|
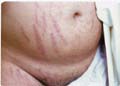
Fig. 248.Drug Reaction,striae
(Corticosteroid)
|
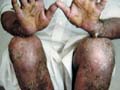
Fig. 249. Drug Reaction
(Exfoliative dermatitis)
|
|
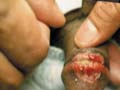
Fig. 250. Fixed Drug Reaction,
(Trimethoprin and sulfa, Bactrim)
|
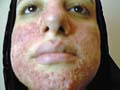
Fig. 251. Drug Reaction, contact dermatitis
(Clindamycine)
|
SPECIAL DRUG
REACTIONS
Fixed drug
reaction. Persistent skin rash that lasts for a long time and recurs
again at the same site when the same drug is taken .
Sulfonamides
and Phenolphthalein besides other drugs can cause this type of
reaction .
Toxic
epidermal necrolysis
This is a
serious reaction especially in young age. Wide spread erythematous
and bullous reaction and desquamation occurs, where the skin surface
separates into sheets. Constitutional symptoms may be severe and the
condition may be fatal .
Sulfonamides,
Butazolidin and Antipyrine are the commonest drugs causing this
syndrome .
Abortion and
fetal abnormalities. Methotroxates may cause such complications .
Stevens-Johnson
syndrome like reaction can be caused by long acting Sulfonamides.
Teeth
changes: Tetracycline taken by pregnant women or given to infants
may lead to hypoplasia of tooth enamel and staining of teeth. The
permanent teeth can be affected in children , with fibrocystic
disease of the pancreas .
Polyneuropathy:
this may be due to large amounts of mercury that is used in topical
preparations and absorbed from the skin surface .
Hemolysis :
the use of sulphones for a long period as in dermatitis
herpetiformis and in treatment of leprosy may lead to blood
hemolysis.
Hearing
problems: due to eight-nerve damage as a result of streptomycin and
colimycin .
Hepatotoxicity:
this can be caused by phenothiazines, methyl testosterone, and
erythromycin osteolate .
Anemia and
hemorrhagic diseases: this is due to bone marrow depression due to
Methotroxates , Grisoefulvin , Butazolidines, Antihistamines,
Novobiocin. Different drugs can cause this problem.
Mucous
membranes changes:
Antibiotics
and vitamin B complex can produce black hairy tongue.
Bismuth
causes the blue stain line along the gums.
Fluorinated
toothpastes may cause cheilitis and ulcerative stomatitis
Skin changes
Glucocorticoids
lead to direct skin atrophy or pigmentary disorders on repeated use
of potent steroids for a long time, especially in infants and young
children .
Certain
inhibitors of lipid synthesis such as ( Triparanol ) lead to
disturbance in keratinization .
Nails .
Declomycin may cause fragmentation of nails .
Hair.
Chemotherapy such as Methotroxates may cause complete hair loss.
Excessive vitamine A intake may cause hair falling.
Pathophysiology of drug reactions
Low molecular
weight drugs such as penicillin cannot induce an immune response at
the beginning of exposure and these are called “ Haptens”. After
repeated intake of such drugs
these haptens bind to endogenous proteins such as serum globulins
forming hapten -protein complex which becomes antigenic causin
production og IgE antibodies in susceptible patients.
Penicillin itself
and the metabolites of penicillin such as penicilloyl, penicilloate
and penilloate may act as haptens.
Combination of
the circulating haptenprotein antigen with IgE antibody bound to the
mast cells and basophils causing cell degranulation through a
calcium – dependent mechanism with release of vasoactive
mediators, producing the anaphylactic state.
The vaso-active
mediators, producing the anaphylaxis state,
include:
Histamine:
secreated by both types of mucosal and connective tissue mast
cells.Histamine produces arteriolar and venous dilation
causing increased vascular permeability.
Prostaglandin
D2 : is secreated
by mast cells only causing peripheral vasodilatation.
Leukotrienes C4 and D4 :is secreated by by both mast cells
and basophils causing
constriction of coronary and peripheral
arterial circulation .These also increase vascular
permeability and
peripheral arterial circulation.
Platelet
activating factor: is secreated by mast cells only , causing
increased vascular permeability and venous dilatation.
Tryptase: the role of mast cells tryptase is unknown .
The other
mediators : are bradykinin producing enzymes, neutral proteases,
cytokines and other substances.
Clinical manifestations of
anaphylaxis
Manifestations
may occur immediately after exposure to the offending drug or after
few minutes.
·
The initial symptoms
include : feeling of warmth or impending doom, flushing, tachycardia
and pruritus.
·
Urticaria is the most common manifestation and may be
accompanied by congestion and swelling of the mucous membranes of
the eyes, nose, mouth,lips and tongue with a feeling of a lump in
the throat which may lead to angioedema of the larynx, epiglotis.
These manifestations may lead to respiratory stridor and
suffocation.
·
Respiratory
manifestations include shortness of breath, tightness in the chest,
acute asthma and wheezing.
·
Cardiac
manifestations include hypotension and cardiac arrest.
·
Neurological
manifestations include loss of consciousness, confusion and
seizures.
·
Gastrointestinal
manifestations: nausea, vomiting and abdominal cramps.
Treatment of
Drug Reaction
A. General
measures
1.
Stop exposure to the drug causing the reaction .
2.
IV normal
physiologic saline for all patients with anaphylaxis.
3.
Maintain airway.
4.
Resuscitation with endotracheal
intubation and advanced cardiac
life support may be necessary in the event of cardiopulmonary
arrest.
B.
Specifc measures
1.
Epinephrine is the treatment of choice in acute anaphylaxis.
Epinephrine
counteracts the vasodilattion , bronchoconstriction ane other
manifestations of IgE mediators released from mast cells and
basophils.
·
Patients presenting with skin rash only and mild
manifestations of anaphylaxis can
be given 0.3 ml of aquous epinephrine 1:1000 subcutaneous route
to an adult or 0.01 mg/kg to a child.
This can be repeated every 15-30 minutes when
required.
·
Shock or cardiac arrest: epinephrine 1:10,000 may be
given IV, as an initial adult
dose of 5-10 ml and can be repeated every 5 minutes as indicated and
according to the patient’s response.
·
Cases with severe hypotension , continuous intravenous
drip of epinephrine may be necessary using the standerd advancec
cardiac life support protocol. The recommended drip dose for adults
is 1 mg of epinephrine 1:1000 dilution or I ml to be added to 500ml
of normal saline, to give a concentration of 2 microgram/ml.
·
Patients with shock may need vasopressor drugs such as
dopamine.
·
In elderly patients
or those under Β-blocker
therapy, 0.5 mg of
glucagon for children or 1 mg for the adults may be indicated and
repeated when required.
·
Oxygen supplemental is often indicated for patients
with cardiac or respiratory symptoms.
·
Asthmatic patients need I.V aminophylline (adult dose
6 mg/kg loading dose over 30 minutes, followed by a maintenance dose
of 0.5 –1 mg/kg/hr).
·
Antihistamines including H1-blockers such as
diphenhydramine (Benadryl) or hydroxazine (Atarax) ,25-50 mg I.V
(for children we give 1 mg/kg I.V.
H2-blockers such as
cemitidine (Tagamet) , 300 mg I.V for adults
and (4mg/kg for children).
·
Corticosteroides such as methylprednisolone (125mg I.V
in adults or 1 mg/kg for children or hydrocortisone(250-500 mg in an
adult of 4-8 mg/kg in children as an initial loading dose may
prevent recurrence of anaphylaxis and bronchospasm.
Sulphonamides Drug Reaction
1.Short acting sulphonamides may
cause :
·
G.I.T irritation such as nausea and vomiting or
·
C.N.S
symptoms such as headache, dizziness, and mental depression.
·
Cyanosis due to formation of sulph-methemoglobinaemia.
·
Allergic skin reaction such as fixed drug eruption,
articaria, and perpura.
·
Severe toxicity may lead to renal damage presenting
with hematouria, oligouria, and anuria.
·
Bone marrow depression leading to anemia and
thrombocytopenia and agranulocytosis.
·
Liver damage leading to toxic hepatitis and jaundice.
·
RBC’s affection causes hemolysis.
·
Hypospermia due to gonadal affection.
·
Toxic polyneuritis and memory disorders.
2.Long acting sulphonamides lead to
:
·
fixed drug reaction and Steven Johnson Syndrome fever
pneumonitis
·
peritonitis and toxic polyneuritis.
Toxic manifestations of
antimicrobial and chemotherapeutic drugs.
·
Hypersensitivity and direct toxicity reaction to
Pencillin and Sulphonamides
·
Anaphylaxis is the common cause of death which is
mainly due to penicillin, sulphonamides, erythrocin and macrolides.
Anaphylaxis is the most common
cause of IgE mediated
anaphylaxis and that is
mainly due to penicillin, followed by B-lactam and others.
Anaphylaxis occurs more commonly after exposure to parenteral
antibiotics.
Hypersensitivity
reactions to antibiotics are due to interaction between the
antibiotic and the immune system.
The
manifestations of Sulphonamides drug reactioins are:
·
Vascultis: These manifestations include small bood
vessels vasculitis .These manifestations are self-limiting and
subside with withdrawal of the drug.
The type of
reaction in sulphamethoxazole is type
1V cell-mediated delayed hypersensitivity reaction.
Clinical finding
in anaphylaxis:
·
Cutaneous manifestations: pruritus, flushing ,
urticaria and angioedema.
·
Cardiovascular manifestations: cardiac arrythmia
and palpitation.
·
Pulmonary manifestations: increased mucous
secreations with rhinorrhea, laryngeal edema, wheezing,
and bronchorrha which causes nasal congestions , hoarseness
,lump of throat, shortness of breath, dyspnea, stridor and
respiratory arrest .
·
General manifestations: conunctival edema
diaphoresis, vomiting ,diarrhea and abdominal cramps.
Hypersensitivity to Macrolides
Erythromycin,
clarithromacin and azithromycin have
usually low immunologic reaction.
Antibiotic poisoning
Mode of poisoning: this is
usually accidental
- Acute:
due to: 1)Overdose
2)Hypersensitivity
- Chronic:
due to: prolonged use.
Toxic manifestations: can be grouped under
the following varieties:
- Allergic
disorders: (mainly due to penicillins in hypersensitive
patients)
1. Mild reaction: skin rash (erythematous,
maculopapular, vesicular,bullous, exfoliative, purpuric, hgic).
2.Severe reaction: generalized anaphylactoid shock and
death.
- G.I.
disorders: (due to chloramphenicol, tetracycline)
1. Irritation of G.I.T.: leading to anorexia, nausea, and
vomiting.
2. Inhibition of
intestinal bacterial flora:
With diminished synthesis of vit.B
complex leading to
inflammation of mucous membrane as (glossitis, stomatitis,
enteritis (diarrhea), colitis, anositis (difficult defaecation),
sore throat.
- Blood
disorders: (due to chloramphenicol, streptomycin).
Inhibition of bone marrow leading to :
1. anaemia
(aplastic).
2. leucopenia (or
agranulocytosis).
3. thrombocytopenia
(with hgic complications).
- Nervous
disorders: (due to streptomycin, neomycin,
chloramphenicol).
1.
8th nerve affection: (by streptomycin)
a.
Auditory symptoms: up to deafness and tinnitis.
b.
Vestibular symptoms: leading to balance disturbances and
vertigo.
2.Grey syndrome: (by chloramphenicol).
It
is due to affection of basal ganglia leading to
peripheral circulatory failure with pallor and cyanosis
(occurs in young infants
and prematures).
- Renal
disorders: (by gentamycin, streptomycin; with poor kidney
function) toxic nephritis, resulting in:
·
Oliguria.
·
Albuminuria.
·
Haematuria.
·
Casts.
- Skin
disorders: Contact dermatitis; during manufacture (allergic
rash…..)
1.Acute
Toxicity (mainly due to penicillins)
Penicillins are used against Gram+ve and Gram-ve organisms.
Penicillins include
benzylpenicillin, phenoxypenicillin, cloxacillin and ampicillin.
Forms of toxicity:
1. Anaphylactic shock: (occurs within seconds to minutes).
In the form of pallor which is followed
immediately by cyanosis, wheezes, pulmonary edema, respiratory
failure and death.
2. Delayed reaction: In the form of:
·
Skin rash.
·
Fever.
·
Pharyngeal and laryngeal edema, respiratory failure
and death.
3.Anaphylactoid reaction:
In the form of :
·
G.I irritation (nausea, vomiting, colic, diarrhea).
·
Convulsions.
·
Pulmonary edema.
2.Chronic
toxicity
A. Tetracyclins:
1. G.I.T.:
a. Irritation…..
b. Inhibition of intestinal bacterial flora…..
2. Kidney:
renal damage due to precipitation of toxic substances.
3. Teeth:
discoloration due to chelation of calcium, this occurs in
children and it is permanent change.
They are broad-spectrum antibiotics used
against systemic infections.
B.
Chloramphenicol:
1.
G.I.T.: upsets leading to diarrhea.
2.
Bone Marrow: depression leading to…..
3.
Grey Syndrome: in infants and prematures.
It is a broad-spectrum antibiotic used in
enteric fever.
C. Erythromycin:
1.
Liver affection: with jaundice.
2.
Allergic manifestations: leading to circulatory failure.
It is used against streptococcal and
pneumococcal infections.
D.
Aminoglycoside antibiotics:
1.
G.I.T.: a. Irritation…..
b. Inhibition of intestinal bacterial flora…..
2.
C.N.S.: 8th nerve affction…..
These antibiotics include streptomycin,
gentamycin, kanamycin, and neomycin.
They are used against Gram-ve bacteria,
(streptomycin is used against T.B. bacilli).
Treatment:
1.
of acute toxicity:
a. Adrenaline S.C.
b. Antihistamines.
c. Corticosteroids I.V.
d. Penicillinase; reverses anaphylactoid and
delay reactions but not anaphylactic one
2.
of chronic toxicity:
a. Stop the drug.
b. For G.I. irritation; milk and bismuth
carbonate.
c. For sore throat and stomatitis; Vit. B complex
and antiseptic measures to mouth.
d.
For bone marrow depression; folic acid and
iron( in mild cases), blood transfusion( in
severe cases).
e. For renal failure; artificial kidney.
REFERENCES
-
Korkij
W, Soltani K. Fixed drug eruption. A brief review. Arch Dermatol
1984; 120: 520-4.
-
Hurwitz
S. Cutaneous disorders of the newborn. In: Clinical Pediatric
Dermatology. Philadelphia; WB Saunders, 1981; 14-15.
-
Meyrick
Thomas RH, Munro DD. Fixed drug eruption due to paracetamol. Br J
Dermatol 1986; 115: 357-9.
-
Hughes
BR, Holt PJA, Marks R. Trimethoprim associated fixed drug
eruption. Br J Dermatol 1987; 116: 241-2.
-
Feinstein A, Sofer E, Trau H et al. Urticaria and fixed drug
eruption in a patient treated with griseofulvin. J Am Acad
Dermatol 1984; 10: 915-17.
-
Commens
C. Fixed drug eruption. Aust J Dermatol 1983; 24: 1-8.
-
Alanko
K, Stubb S, Reitamo S. Topical provocation of fixed drug eruption.
Br J Dermatol 1987; 116: 561-7.
-
Guin
JD, Haynie LS, Jackson D et al. Wandering fixed drug eruption: A
mucocutaneous reaction to acetaminophen. J Am Acad Dermatol 1987;
3: 399-402.
-
Alanko
K, Stubb S, Reitamo S. Topical provocation of fixed drug eruption.
Br J Dermatol 1987; 116: 561-7.
-
Andersen KE, Maibach HI. Allergic reaction to drugs topically.
Clin Toxicol 198 0; 16: 415-65. Angelini C, Vena CA, Meneghini CL.
Contact allergy to antiviral agents. Contact Derm 1986; 15:
114-15.
-
Bandmann H-J, Calnan CD, Cronin E et al. Dermatitis from applied
medicaments. Arch Dermatol 1972; 106: 335-7.
-
Beck
MH, Burrows D, Fregert S et al. Allergic contact dermatitis to
epoxy resin in ostomy bags. Br J Surg 1985; 72: 202-3.
-
Burry
JN, Hunter CA. Photocontact dermatitis from Jadit. Br J Dermatol
1970; 82: 224-9.
-
Calnan
CD. Diethyldithiocarbamate in adhesive tape. Contact Derm 1978; 4:
61.
-
Calnan
CD, Cronin E. False positive reaction to mercaptobenzo-thiazole
from rubber in eyedrop bottle. Contact Derm 1981; 7: 283-4.
-
Calnan
CD, Frain-Betl W, Cuthbert JW. Occupational dermatitis from
chlorpromazine. Trans St John‘s Hosp Dermatol Soc 1962; 48:
49-74.
-
Clark
EW, Blondeel A, Cronin E et al. Lanolin of reduced sensitizing
potential. Contact Derm 7: 80-3.
-
Colver
CB, Inglis JA, McVithe E et al. Dermatitis due to intravesical
mitomycin C: a delayed-type hypersensitivity reaction? Br J
Dermatol 1990; 122: 217-24.
-
Coopman S, Dooms-Coossens A. Cross-reactions in topical
corticosteroid contact dermatitis. Contact Derm 1960; 19: 145-6.
-
Cronin
E. Contact Dermatitis. Edinburgh: Churchill Livingstone 1980:
192-278.
-
Cronin
E. Contact Dermatitis. Edinburgh: Churchill Livingstone, 1980:
805-13 and 832-8.
-
Curley
RK, Macfarlane AW, King CM. Contact sensitivity to the amide
anaesthetics lidocaine, prilocaine, and mepivacaine. Arch Dermatol
1986; 122: 924-6.
-
Dahlquist I, Fregert S, Cruvberger B. Detection of formaldehyde in
corticoid creams. Contact Derm 1980; 6: 494.
-
Shoss
RG, Rayhanzadeh S. Toxic epidermal necrolysis following measles
vaccination. Arch Dermatol 1974; 110: 766-70.
-
Roujeau J-C, Guillaume J-C, Fabre J-P et al. Toxic epidermal
necrolysis (Lyell syndrome). Incidence and drug etiology in France
1981-1985. Arch Dermatol 1990; 126: 37-42.
-
Revuz
J, Roujeau J-C, Guillaume J-C et al. Treatment of toxic epidermal
necrolysis. Cretail‘s experience. Arch Dermatol 1987; 123:
1156-8.
-
Lyell
A. Toxic epidermal necrolysis (the scalded skin syndrome). Br J
Dermatol 1979; 100: 69-86.
-
Heimbach DM, Engrav LH, Marvin JA. Toxic epidermal necrolysis. A
step forward in treatment. J Am Med Assoc 1987; 257: 2171-5.
-
Barnes
RL, Wilkinson DS. Epidermal necrolysis from clothing impregnated
with paraffin. Br Med J 1973; iv: 466-7.
-
De
Groot AC, Conemans JMH. Contact allergy to furazolidone. Contact
Derm 1990; 22: 202-5.
-
Deschamps
D, Carnier R, Savoye J et al. Allergic and irritant contact
dermatitis from diethyl-betachloroethylamine. Contact Derm 1988;
18: 103-5.
-
Van
Dijk E, Neering H, Vit?nyi BEJ. Contact hypersensitivity to sesame
oil in patients with leg ulcers and eczema. Acta Derm Venereol
1973; 53: 133-5.
-
Dohn W.
Beitrag zur Frage der Chloramphenicol-Kontaktallergien. Hautarzt
1965; 16: 174-7.
-
Allergenicity prediction and pharmacopoeial requirements. Contact
Derm 1983; 9: 175-85, and 352-9.
-
Dooms-Goosens
A, Degreef H, Coopman S. Corticosteroid contact allergy: a
reality. In: Frosch
-
PJ,
Dooms-Coossens A, Lachapelle J-M et al., eds. Current Topics in
Contact Dermatitis. Berlin: Springer, 1989: 233-7.
-
Dooms-Coossens A, Degreef H, Vanhee J et at. Chlorocresol and
chloracetamide: allergens in medications, glues and cosmetics.
Contact Derm 1981; 7: 51-2.
-
Fisher
AA. Contact Dermatitis, 3rd edn. Philadelphia: Lea and Febiger,
1986: 141-257.
-
Fisher
AA. Unnecessary addition of ethylenediamine hydrochloride to
‘generic‘ nystatin creams. J Am Acad Dermatol 1989; 20:
129-30.
-
Fregert S, M?ller H. Photo cross-sensitization among
halogen-hydroxybenzoic acid derivatives. J Invest Dermatol 1964;
43: 271-4.
-
Fregert S, Trulson L, Zimerson E. Contact allergic reactions to
diphenylthiourea and phenylisothiocyanate in PVC adhesive tape.
Contact Derm 1982; 8: 38-42.
-
Gelfarb M, Leider M. Allergic eczematous contact dermatitis.
Report of a case caused by sensitization to undecylenic acid and
its zinc salt. Arch Dermatol 1960; 82: 642-3.
-
Gellin
GA, Maibach HI, Wachs CN. Contact allergy to tolnaftate. Arch
Dermatol 1972; 106:
-
Goh CL.
Contact sensitivity to proflavine. Int J Derm 1986; 25: 449-51.
-
Cola
M, Francalanci S, Brusi C et at. Contact sensitization to
acyclovir. Contact Derm 1989; 20:
-
C?ransson
K, Lidبn S. Contact allergy to sorbic acid and unguentum
Merck. Contact Derm 1981; 277.
-
Harris
GL, Maibach HI. Allergic contact dermatitis potential of 3
pyridostigmine bromide transdermal drug delivery formulations.
Contact Derm 1989; 2l: 189-93.
-
Hannuksela
M, Piril? V, Salo OP. Skin reactions to propylene glycol. Contact
Derm 1975; 1:
-
Hausen
BM, Heesch B, Kiel U. Studies on the sensitizing capacity of
imidazole derivatives. Am J Contacf Derm 1990; 1: 25-33.
-
Hausen
BM, Wollenweber E, Senff H et al. Propolis allergy (1) Origin,
properties, usage and literature review. Contact Derm 1987; 17:
163-70.
-
Hjorth
N, Trolle-Lassen C. Skin reactions to ointment bases. Trans St
John‘s Hosp Dermatol Soc 49: 127-40.
-
Holdiness M. A review of contact dermatitis associated with
transdermal therapeutic systems. Contact Derm 1989; 20: 3-9.
-
Jelen
C, Tennstedt D. Contact dermatitis from topical imidazole
antifungals: 15 new cases. Contact Derm 1989; 21: 6-11.
-
Jordan
WP. Cross-sensitization patterns in acrylate allergies. Contact
Derm 1975; 1: 13-15.
-
Dooms-Goossens A, Degreef H. Contact allergy to petrolatums. (I)
Sensitizing capacity of different brands of yellow and white
petrolatums. (II) Attempts to identify the nature of the
allergens.
-
Jones
SK, Kennedy CTC. Contact dermatitis from tioconazole. Contact Derm
1990; 22: 122-3.
-
Katz
BE, Fisher AA. Bacitracin: a unique topical antibiotic sensitizer.
J Am Acad Dermatol 1987; 1016-24.
-
Kinnunen T, Hannuksela M. Skin reactions to hexylene glycol.
Contact Derm 1989; 21: 154-8.
-
Kligman AM. Lanolin allergy: crisis or comedy? Contact Derm 1983;
9: 99-107.
-
Lachapelle JM, Lamy F. On allergic contact dermatitis to
virginia-mycin. Dermatologica 1973; 320-2.
-
Larsen
WG. Allergic contact dermatitis to the perfume in Mycolog cream. J
Am Acad Dermatol 1: 131-3.
-
Levine
BB. Studies on the mechanism of the formation of the penicillin
antigen. I. Delayed allergic cross-reactions among penicillin C
and its degradation products. J Exp Med 1960; 112:
-
Leyden
JJ, Kligman AM. Contact dermatitis to neomycin sulfate. J Am Med
Arsoc 1979; 242:
-
Lovell
CR, Staniforth P. Contact allergy to benzalkonium chloride in
plaster of Paris. Contact Derm 1981; 7: 343-4.
-
Meneghini CL, Rantuccio F, Lomuto M. Additives, vehicles and
active drugs of topical medicaments as causes of delayed-type
allergic dermatitis. Dermatologica 1971; 143: 137-47.
-
Menné
T, Hjorth N. Rouhne patch testing with paraben esters. Contact
Derm 1988; 19: 189-91.
-
Nater
JP, de Groot A.C. Unwanted Effects of Cosmetics and Drugs used in
Dermatology, 2nd edn. Amsterdam: Elsevier, 1985: 44-108 and
passim.
-
Neumann RA, Knobler RM, Lindemayr H. Tiaprofenic acid induced
photosensitivity. Contact Derm 1989; 20: 270-3.
-
Patruno C, Auricchio L, Mozzillo R et at. Allergic contact
dermatitis due to tromantadine hydrochloride. Contact Derm 1990;
22: 187.
-
Puig
L, Abadias M, Alomar A. Erythroderma due to ribostamycin. Contact
Derm 1989; 21:
-
Rajka
C, Pallin 0. Sensitization to locally applied Antastene. Acta Derm
Venereol 1964; 44:
-
Reitamo S, Lauerma AI, F?rstr?m L. Detection of contact
hypersensitivity to topical corticosteroids with
hydrocortisone-l7-butyrate. Contact Derm 1989; 21: 159-65.
-
Reynolds NJ, Harman RRM. Allergic contact dermatitis from
chlorhexidine diacetate in a skin swab. Contact Derm 1990; 22:
103-4.
-
Takahashi M, Matsuo I, Ohkido M. Contact dermatitis due to
honeybee royal jelly. Contact Derm 1983; 9: 452-5.
-
Salo
OP, Piril? V, Viljanen E. Sensitivity to topical dequaline. Acta
Allergol 1968; 23: 490-6.
-
Schwartz BK, Glendenning WE. Allergic contact dermatitis from
hydroxypropyl cellulose in a transdermal estradiol patch. Contact
Dermatitis 1988; 18: 106-7.
-
Shelley WB, Heaton CL. Minocycline sensitivity. J Am Med Assoc
1973; 224: 125-6.
-
Briggs
GG, Freeman RK, Yaffe SJ. Drugs in Pregnancy and Lactation.
Baltimore: Williams & Wilkins, 1986.
-
Lenz W.
Malformations caused by drugs in pregnancy. Am J Dis Child 1966;
112: 99-106.
-
Miller
ME, Seals J, Kaye R et al. A familial, plasma-associated defect of
phagocytosis. Lancet 1968; ii: 60-3.
-
Vujasin J, Petrovic D. Biotin in some erythemato-squamous
dermatoses of babies. Dermatologica 1952; 105: 180-3.
-
Shono
M, Hayashi K, Sugimoto R. Allergic contact dermatitis from
croconazole hydrochloride. Contact Derm 1989; 21: 225-7.
-
Tennstedt
D, Lachapelle J-M. Allergic contact dermatitis to 5-fluorouracil.
Contact Derm 1987; 279-80.
-
Valsecchi
R, Cainelli T. Contact dermatitis from ibuproxam. A case with
cross-reactivity with ketoprofen. Contact Derm 1990; 22: 51.
-
Van
Ketel WC. Systemic contact-type dermatitis by derivatives of
adamantane. Dermatosen 1988; 23-24.
-
Wasilewski C. Allergic contact dermatitis from nystatin. Arch
Dermatol 1970; 102: 216-17.
Top
|