|
PRURIGO
|
|
|
|
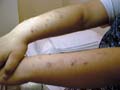
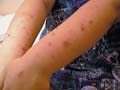
Prurigo is characterized by the prurigo papule that is dome-shaped and topped with a small vesicle, which usually appears as an excoriated lesion due to severe scratching. The crusted papules are usually seen rather than the primary papule with its topped vesicle. Types of Prurigo The most common types of prurigo are: 1. Prurigo simplex 2. Prurigenous dermatoses
This type of prurigo appears usually in middle-aged individuals and in both sexes .The common sites involved are extensor surface of the extremities, trunk, face and scalp. Clinical Feature The clinical picture is variable, where the prurigo papules are present as flat-topped surmounted by vesicles, excoriated papules or in the form of lichenified pigmented skin lesion simulating neurodermatitis or dermatitis herpetiformis.
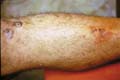
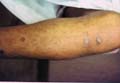
Different clinical varieties of prurigo Chronic prurigo of adults is a poorly defined entity that mimics the widespread papular urticaria of insect bites. The cause is unknown although emotional stress seems to be a contributory factor in some cases. Insect bites especially after repeated exposure in susceptible persons may play an important role. The disorder is more common in adults, with an onset in the spring and summer months. The characteristic lesions are found on the trunk and neck, and present as itchy red papules which occasionally coalesce to a reticular pattern, and reticular hyperpigmentation. Prurigo of this type occasionally occurs with malignant disease, especially Hodgkin‘s lymphoma and in polycythaemia. Clinical Manifestations Prurigo is considered as one of the most common skin diseases, which causes severe and sometimes intolerable itching, especially in emotionally unstable individuals. The eruption consists of small, irritable papules, usually most numerous on the extensor aspects of the limbs, the upper trunk and the buttocks with very variable distribution. Nodular prurigo may appear on the scalp as a separate lesion or as a part of the disease affecting other parts of the body. Nodular prurigo of the scalp is not easily differentiated from neurodermatitis. The course may be continuous for months or years or there may be partial or complete remissions. The individual lesion is a hard globular nodule, 1-3 cm in diameter, with a raised warty surface. The early lesion is red and may show a variable urticarial component, but all the lesions tend to be pigmented. Crusting and scaling may cover recently excoriated lesions. There is an irregular ring of hyperpigmentation immediately around the nodules. The lesions are usually grouped. New nodules develop from time to time, but existing nodules may remain pruritic indefinitely although some may regress spontaneously to leave scars. The disease runs a very long course Diagnosis The large, more or less symmetrical nodules and the intense pruritus usually establish the diagnosis. Differential Diagnosis
These are different diseases associated with pruritus and papular lesions where some is accompanied by wheals, eczematization and lichenifecation. Different clinical types of prurigo Besnier‘s prurigo: This is chronic lichenified flexural lesions and is considered as a type of atopic dermatitis. Fig.293b. Besnier's prurigo Hutchinson‘s summer prurigo: this is an actinic type precipitated by excessive exposure to sunlight. Prurigo Chronica Multiformis: presents with prurigo nodules, lichenification, eczematization, enlarged lymph nodes and esinophilia. Hebra‘s prurigo - Hebra‘s prurigo is now rarely diagnosed and its status is questionable. Most cases occurred in atopic subjects and the role of poor nutritional and hygienic conditions were considered as predisposing factors. The possibility that some cases represent papular urticaria modified in an atopic subject must be considered. The treatment is that of atopic dermatitis. Prurigo mitis : This type begins early in childhood and is characterized by uniform type of small rounded, flesh colored or erythematous, severely pruritic, flat-topped papule, surmounted by a vesicle. Severe itching lead to excoriation, eczematization and on healing of lesions, they may leave skin scarring. Prurigo pigmentosa: The disorder is more common in adults, with an onset in the spring and summer months. The characteristic lesions are found on the trunk and neck, and present as itchy red papules that occasionally coalesce to a reticular pattern. Later they are superseded by a reticular hyperpigmentation. Treatment Dapsone: The skin lesions and pruritus responds dramatically to Dapsone. Minocycline This is the drug of choice for adults. The recommended daily dose is 200mg. It is expected to clear the skin lesion within a few days. Prurigo Agra This type may show familial tendency with a history of allergic reactions. Clinical Features Hard, excoriated prurigo papule associated with lichenifecation. Secondary infection is common. Pustulation and pitted scars are common manifestations due to the severe scratching and excoriation of the lesion. Etiology of Prurigo
Differential Diagnosis Dermatitis herpetiformis Neurodermatitis Chronic atopic dermatitis Herpes gestationis Treatment Local applications are of little value. Avoid irritating substances, insect bites, avoid over heating or exposing the skin to cold. Intralesional injection of the nodules with a steroid such as triamcinolone is often helpful. Antihistamines: Zyrtec10mg and Atarax, 25mg and 100mg may help in relieving itching. Tranquilizers: may be of great help especially in emotionally disturbed individuals. Higher doses can be given at night, where itching is more in some patients due to skin heating especially in wintertime. Depot corticosteroids (Depot medrol or Kenalog 40mg) can be given every 2-4 weeks. Benoxaprofen have also been used with success in some cases. Thalidomide is probably the most effective treatment, if it is not contra-indicated by the risk of pregnancy, though there is always some risk of painful neuropathy.
|
| Contents | << Previous Chapter | Next Chapter >> | Search |