|
DISEASES OF THE MUCOUS MEMBRANES
|
|
|
|
Mucous patches of the mouth should not be mixed with milk patches in babies due to accumulation of milk on the inner sides of the buccal mucosa. Vesicles or bullae leave a grayish erosion after ulceration, while papular lesions which may be significant on the skin surface become difficult to differentiate in the mucous membranes of the mouth. Usually mouth lesions are whitish, macerated and soft. Different physiological or pathological factors may affect the buccal and tongue mucosa. Some of the diseases of mucous membrane, which accompany skin diseases were already discussed in the previous chapters.
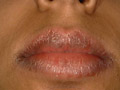
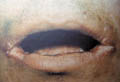
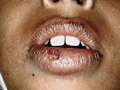
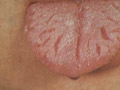
CHEILITIS Cheilitis is caused by different factors, which may be allergic or inflammatory. The lower lip is the most common affected. The lesion may be localized in the lip or may extend to the adjacent mucocutaneous or even to the skin of the face. Fig. 372 Cheilitis &Glossitis Etiology of Cheilitis
The different factors, which may lead to glossitis and stomatitis include the following: Malnutrition Lack of proper hygiene of the mouth Vitamin deficiency mainly vitamin C and B complex. Clinical Features The ulcers are punched out, covered by dirty white pseudomembrane covering the mucous membranes of the tongue, lips, buccal mucosa, tonsils, and the pharynx and may involve the whole respiratory tract mucosa. Fig.381b. Glossitis Herpetic gingivostomatitis Children and young age groups are commonly infected with herpes virus leading to herpetic lesions of the mouth, tongue and lips. Painful ulcerations are common which may interfere with feeding and increased salivation. Gangrenous stomatitis Gangrenous stomatitis occurs in children with poor nutrition, lowered resistance and improper dental hygiene. The lesions manifest with mucosal ulcerations of the mouth and genitalia, which rapidly becomes gangrenous. The condition may extend to the adjacent tissues and may be extensive involving the bones and may be fatal. Treatment Proper hygiene of the mouth and correction of the predisposing factors. Mild mouth wash antiseptics. Tetracycline suspension orally. This should be kept for few minutes in the mouth to have a local effect. Care should be taking when treating babies or young children with Tetracyclines. Another oral antibiotic suspension such as Zithromax can be substituted for young age groups. Systemic antibiotics.
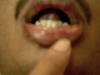
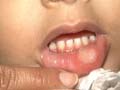
The lesions are recurrent, tender, small shallow erosions surrounded by an erythematous zone affecting the buccal mucosa. These may interfere with feeding and speech. It is believed that streptococcus infection may be the causative of recurrent aphthus stomatitis.
Fig. 381b. Aphthous stomatitis The lesions may appear also on the genitalia and has to be differentiated from other diseases of these areas such as viral, fungal and Behcet‘s disease. Recurrence of lesions may be predisposed by: Lower body resistance. Emotional and psychic trauma. Trauma: self-biting, hard, harsh toothbrushes and other tools used for cleaning of the mouth and teeth. Hormonal changes. Allergy to certain types of foods and additives such as tartrazine. Drug reaction. Infections such as herpes virus infections may predispose to recurrence. Differential Diagnosis It is usually not easy to differentiate such condition from other diseases affecting the buccal mucosa: Candidiasis Herpes simplex infections Vincent‘s angina Mucous patches of syphilis Vitamin deficiency mainly scurvy and pellagra. Behcet‘s disease Pemphigus Fig.381c. Pemphigus Lichen planus Treatment General measures Treatment of the predisposing factors. General hygiene of the mouth and teeth. Avoid strong mouth antiseptics Avoid mouthwashes containing allergenic substances. Avoid contact with certain foods such as citrus, spicy and harsh foodstuffs. Local treatment Non-specific medications: Different local applications were used with variable results. Tetracycline suspension especially if kept in the mouth few minuets before swallowing, may give good results in some cases. Xylocaine viscous 2 % (Lidocaine) may be used especially in painful conditions few minuets before feeding for infants and children. Local topical steroid (Kenalog orabase) or prednisone lozenges may be used if viral or bacterial infections are excluded. Lesions of the inner sides of lips can be touched gently by swab moistened with salicylic acid 3% and lactic acid 4 % prepared in flexible collodion .
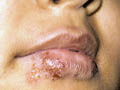
RECURRENT HERPES SIMPLEX OF THE MOUTH
Diagnosis Typical clinical picture, which includes painful, grouped vesicles or ulcerations on an erythematous base. Tzank test: scrapings from the base of the ulcers stained with Wright‘s stain show the multinucleated giant cells. Immunoflorecent tests are diagnostic.
This is a viral disease caused by Coxsackie virus affecting mainly children especially in summer time. Modes of Infection It is believed that certain species of flies can transmit the disease. Direct infection from infected individuals. Clinical Manifestations General manifestations Fever, which may be high, headache, sore throat, anorexia and dysphagia. Skin manifestations Skin lesions may appear in different forms mainly: Exanthematous reaction. Urticarial lesions. Pruritic macules. Mucous membranes manifestations: Minute papules, vesicles and ulcers surrounded by an erythematous areola appear on the mucous membrane, which are characteristically apparent on the pharynx, tonsils and throat .The lesions appear usually in small groups, which may coalesce and ulcerate. The ulcers are shallow, grayish yellow and punched.
BEHCET‘S
DISEASE Behcet‘s syndrome is characterized by:
Clinical Features Skin manifestations Skin lesions may be: Erythema nodosum Erythema multiforme Acniform eruption Papulo -pustules, subungual abscess and pyoderma. General manifestations: Thrombophlebitis Arthritis: polyarthritis. Cerebellar syndrome resembling multiple sclerosis. Mucous membrane manifestations Mucous membrane lesions are single or multiple with dirty grayish base surrounded by red halo. Mucous membrane of the buccal mucosa, palate, lips and tongue may be involved. Ulcerations may leave scarring The ulcers are tender and cause severe pain that may interfere with eating, speech and gives a foul smell of the mouth. Genital manifestations Ulceration of the scrotum, penis and urethra. Ulceration of labia, vagina and cervix. Ulceration of the anal area, crural areas and perineum. The ulcers are extremely painful. Healing of ulcers may lead to scarring and deformities. Eye manifestations Severe peri-orbital pain and photophobia. Conjunctivitis, hypopyon, iritis, iridocyclitis. Blindness may be the end stage due to optic nerve atrophy.
This syndrome occurs chiefly in young males and may affect children. Clinical Features This syndrome is characterized by triad manifestations: Eye: Conjunctivitis, iritis, and keratitis. Urethritis: Non-bacterial, painful and bloody urination and pyuria. Cystitis, prostatitis and seminal vesiculitis are common Arthritis: Swollen and tender joints. General manifestations: Fever, weakness and weight loss. Skin manifestations: Multiple small, yellowish vesicles and ulcers on the palms and soles. Lesions of the palms and soles become thickly hyperkeratotic and crusted resembling keratoderma blenorrhagica. Mucous membrane manifestations: Mucous membrane lesions are superficial ulceration of the genitalia and mucous membranes of pharynx and hard palate. Cardiac manifestations: are rare manifestations of the disease. Endocarditis, myocarditis, pericarditis and aortic insufficiency are uncommon manifestations.
Dryness of the mouth may be due to different local or systemic factors. Etiology
Etiology
Cytotoxic drugs. Phenothiazines. Anticonvulsants. Chloropromazine: may cause purple or yellowish brown pigmentation of the skin and mucous membranes. Minocycline: may produce blue-gray gingival pigmentation. Heavy metals.
This syndrome is characterized by pigmentation and intestinal polyposis. The pigmented macules may be present at birth and usually appear in infancy and early childhood, but may develop later in life. The oral mucous membrane is almost constantly involved. The oral pigmentation is usually permanent, but the macules on the lips and skin may fade after puberty. Rarely, the nails may be pigmented, diffusely or in longitudinal bands. Clinical Features Mucous membrane manifestations Round, oval or irregular patches of brown or almost black pigmentation 1-5 mm in diameter are irregularly distributed over the buccal mucosa, the gums, the hard palate and the lips, especially the lower. Mucosal and facial pigmentation without evidence of intestinal polyposis may be found in relatives. Intestinal polyposis may cause repeated bouts of abdominal colic, vomiting, intussusceptions, malignancy and rectal bleeding. Skin manifestations The pigmented macules on the face are smaller, dark often under 1 mm and are concentrated around the nose and mouth. Larger macules may be present on the hands, feet, palms and soles. Systemic manifestations Abdominal pain is usually caused by intestinal obstruction. Rectal bleeding is common and haematemesis may occur with gastric or duodenal polyps. Anemia. Differential Diagnosis Addison‘s disease Skin freckling Gardner‘s syndrome
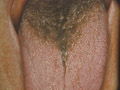
WHITE PATCHES OF THE BUCCAL MUCOSA Different factors may cause white patches of the buccal mucosa. Etiology: Infections: of the buccal mucosa such as herpetic lesions may cause white patches surrounded by an erythematous area. Thrush: produces oral white patches. Mucous patches of syphilis: Grayish white painful patches, slightly elevated and surrounded by an erythematous area. The buccal lesions occur most frequently on the inner lower lips, tongue and other parts of the mouth. The mucous patches are highly contagious and serological tests of syphilis are positive. Lichen planus. Pemphigus Benign mucosal pemphigoid Hairy leucoplakia: is a white lesion that appears on the tongue and whitish flaky pseudomembrane on an erythematous base. Culture will reveal the causative organism. Leucoplakia: lichenoides lesions are associated with various drugs, liver disease or graft-versus-host disease. White sponge nevus: white, thickened spongy patches appear on the inner sides of lips, cheeks and sides of the tongue Carcinoma may present as a white lesion. Dyskeratosis congenita causes white patches
Etiology
Cacogeusia (an unpleasant taste in the mouth) and halitosis are caused by different factors mainly: Etiology
Etiology
|
| Contents | << Previous Chapter | Next Chapter >> | Search |