|
Hair is derived from the epidermis . It develops about the third or
fourth month of the fetal life. After birth the hair follicles
distributed on the scalp or other parts of the body become stable
and no more hair follicles are developed after that. Meanwhile hair
follicles may be modified or decreased in number by age or due to
different factors .
There are
two types of skin, the glabrous type, which is covered by hair, and
non-glabrous, which is the smooth skin, not covered by hair even
after puberty.
Newborn
babies skin is covered by fine light colored hair known as lanugo
hairs, which tend to be most dense on the face, limbs and trunk.
Lanugo hair is shed during the first months of life to be replaced
by vellus hair.
Different
types of hair:
The lanugo
hair:
It is fine
hair, lightly pigmented, which covers most of the whole skin surface
except palms, soles and the red surface of the lip near the
mucocutaneous junction.
The vellus
hair:
This is fine
hair, usually light colored and is characteristically seen on
children face and limbs. The vellus hair usually covers the female
skin .
The terminal
hair:
This is
coarse, thick and pigmented hair. The hair follicle may produce a
vellus hair at the beginning where later, under certain factors it
7 is transformed into terminal hair.
The type of
hair varies according to the site, sex, race, age and other factors
mainly the sex hormones.
HAIR GROWTH
CYCLE
Development
and distribution of hair follicles.
Hair
follicles appear first in the regions of the eyebrows, upper lip and
chin at about 9 weeks of embryonic development, and in other regions
in the fourth month . Hair follicles of the scalp are established
after about six months after birth.
The total
number of follicles in an adult man has been estimated at about 5
million, of which about 1 million are in the head (face, eyebrows,
moustache area, eyelids).
Hair cycle
The growth
of hair occurs in cycles. Hair does not continue to grow
indefinitely. Hair follicles grow in a repetitive sequence called
hair cycle. Hair growth is present in different stages and in
special balance in normal individuals, where the growing hairs
constitute the majority.
|
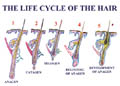
Fig. 406. Hair Cycle |
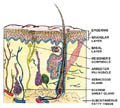
Fig. 407. Structure of skin and its appendages |
-
Anagen
(growing phase):
This is the
growing phase which takes about 3 months or more depending on the
site. The follicular cells grow, divided and become keratinized to
form growing hair. The base of the hair shaft is moist and soft
where a darkly pigmented portion is evident just above the hair
bulb. The growing hair in normal individuals constitutes about 90%
of the total hair .
-
Telogen
(resting phase):
Telogen
hairs are in a state of resting (for about 3 months)where part of
the growing hair (about 10 % )passes in this stage before falling .
Telogen hair
is also known the “club hair“ that is shed when a new hair
grows.
-
Catagen
(transition phase):
Catagen
hairs undergo transition from growing to the resting phase where
growth ceases with the formation of club hair .
When the
hair approaches the end of its growing phase different changes
occur in the follicle.
Under normal
conditions most of the hair is in the growing phase , others in the
resting phase, and a small percentage of hair is in the catagen or
falling phase.
Normal scalp
has approximately 100,000 follicles. Scalp hair growth is 0.35 mm/
day.
The growing
period of the scalp hair is about six months.
The growing
phase is much altered by different factors, mainly hormonal,
generalized debilitating diseases, stress, pregnancy, lactation and
other factors. In such conditions the growing phase is shortened and
most of the hair pass in the resting phase.
The scalp
hair normally looses from 100-120 hairs / day . The lost hair is
compensated later on.
In contrast
to the belief by some individuals, mainly females, that baldness is
expected because she looses that number of hair daily. The
convincing answer is that if this is the case and falling hairs are
not replaced by new hair, all human beings are bald.
Resting hair
is exposed to falling easily because, they are less firmly anchored
.
Scalp hair
differs in that its growth does not require any androgenic stimulus,
in contrast increased circulating androgens may lead to hair
falling.
STRUCTURE OF
HAIR
The hair is
composed of :
Hair shaft
or stem which forms at the lower end; the hair papilla. The
hair shaft is made up of keratinized cells. The hair shaft consists
of the sheath or cuticle, the cortex and the medulla.
The medulla begins at some distance from the tip and ends near the
bulb. The hair follicle may in fetal life produce lanugo hair and in
the adult life the terminal hair .
|
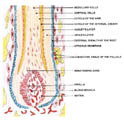
Fig. 408. Hair Structure |
The hair
root or matrix that is the intrafollicular portion of the bulb.
Outside the
hair root is the hair cuticle . The inner root sheath is made up of
the cuticle and additional two layers of cells , the Huxley and the
Henele layer . The outer root sheath extends from the epidermis to
the hair bulb. It is thickened near the epidermis and becomes
attenuated in its lower portion. The sebaceous gland is derived from
it .
The hair
bulb is an expanded mass of epithelial cells, which gives to
different types of keratinized cells. The bulb and part of the shaft
are contained in the hair follicle
COLORS OF
HAIR
Hair color
depends on the degree of melanin synthesis in the matrix fibers and
the intervening spaces between the fibers.
Melanin
synthesis begins in the matrix fibers. Melanin in the hair follicle
is produced in the cytoplasm of melanocytes .
The pigment
in dark and gray color of the hair is composed of tyrosine - melanin while the blond and red hair, the pigment is phenoalanin.
Black hair
color - In this type
the melanocytes contain dense melanosomes.
Brown hair :
melanocytes are smaller.
Light brown
hair : consists of
mixture of the melanosomes of the dark hair and the incomplete
melanosomes of the dark hair.
Red hair :contains
iron pigment. Melanin deposit is incomplete on the matrix fibers
Grey hair :
Melanogenic activity is decreased.
Melanocytes
and melanosomes are decreased.
Loss of
tyrosinase activity.
Factors
affecting hair color.
Age
Race
Metabolic
changes
: such as in
porphyrias and kwashiorkor disease .
Drugs:
chloroquine therapy for a long time may cause depigmentation of
hair. Chloroquine interferes with phaeomelanin synthesis. The
reaction is usually reversible where the color returns back to normal within
few months after stopping the drug .
Topical
preparations:
Dithranol and chrysarobin stain light colored or gray hair mahogany
brown. Resorcin formerly used a great deal in a variety of skin
diseases, colors black or white hair yellow or yellowish-brown.
Mephenesin,
glycerol ether used for diseases with muscle spasms, causes
pigmentary loss in dark-haired people .
Triparanol,
an anticholesterolaemic drug and fluorobutyrophenone, an
antipsychotic drug can cause change in the hair color.
Minoxidil
and diazoxide, two potent anti hypertensive agents, both cause
hypertrichosis and darkening of hair.
Diazoxide
causes reddish hair discoloration, whilst Minoxidil darkens hair
mainly by converting vellus hair to terminal hair.
Hydroquinone
and phenylthiourea interfere with tyrosine activity, causing
hypopigmentation of skin and hair .
HAIR DISEASES
In this
chapter short notes are mainly applied to the most common diseases
and abnormalities of hair in infants and children ,where some of
these diseases and changes may be the same as in older age groups.
|
ALOPECIA
AREATA
Alopecia is
a localized or generalized loss of hair related either to follicular
dysfunction or follicular destruction.
There are
different types of alopecia related mainly to the cause.
|
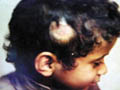
Fig. 409. Alopecia Areata
|
Clinical
Features
The patches
are oval or round where at the periphery there is loose hair were
given the term “exclamation mark.” When pulled shows an atrophic
hair bulb. The scalp surface of the area is usually smooth.
The hair
loss may continue spreading peripherally forming new areas free of
hair, or regeneration may occur later on. The new growing hair is
downy, light or even white in color devoid of pigment.
In long
standing cases of alopecia, fingernails stibbling may occur.
Etiology of
alopecia
Local
infection of the scalp such as folliculitis , Tinea capitis and
favus.
-
Skin
diseases: Lichen planus, discoid lupus erythematosus.
-
Focal
infection :
-
Chronic
tonsillitis, sinusitis and septic foci have blamed as a causative
for alopecia.
-
Dental
abnormalities :
Infections
of teeth
Dental
caries in children, errors of refractions and impacted wisdom
tooth in older age groups are some of the different causes of
alopecia areata .
-
Stress,
nervous tension and psychic trauma are also considered important
causes of alopecia areata.

Fig.410b. Alopecia and nail dystrophy
Majority
cases of alopecia areata we face in our practice in children are due
to dental caries , psychic trauma, septic foci in the tonsils or
sinuses and due to immunological factors.
|
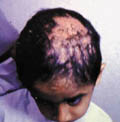
Fig. 410. Cicatrical Alopecia |

Fig. 411. Alopecia Totalis |
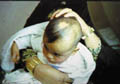
Fig. 412. Congenital Alopecia |
OTHER TYPES
OF ALOPECIA
-
Traction
Alopecia
This is
common in young girls in the school age where the mother after
combing the hair,
pull strongly and fixing the hair to the side
directions or to the back making what is called “ the horse tail“.
By time this continuous and repeated traction will cause frontal
regression of the hair and present later on with alopecia .
|

Fig. 413. Traction Alopecia |
-
Pressure
Alopecia :
This may be
noticed in babies who sleep most of the time on the occipital region
where by continuous pressure on the occipital area, localized patch
free of hair develops.
|
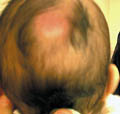
Fig. 414. Pressure Alopecia |
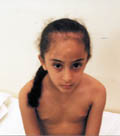
Fig. 415. Traction Alopecia |
It is
important to instruct mothers to change from time to time the
sleeping position of the baby and if necessary to put a pillow on
one of his sides to keep the baby at that steady position during sleeping .
-
Alopecia
in the course of febrile diseases
Alopecia
may develop during systemic diseases such as fevers and chronic
recurrent bacterial infections.
-
Telogen
effluvium (Disturbances of hair cycle)
Telogen
effluvium is the early and excessive loss of normal hairs from
normal follicles of the scalp. This type of hair loss is most
common in females that may occur in the postpartum period, post
febrile, postnatal , post surgery and post-traumatic conditions.
Increased
shedding of hair is clearly related to the stressful episode that
preceded hair falling by 6-16 weeks.
|
Plucked
hairs show a large proportion of normal clubs until the shedding
is complete.
Telogen
effluvium is always diffuse and never total .
-
Nutritional alopecia
Malnutrition
influences the growth, structure of the hair shaft and sometimes,
the color of the hair.
|

Fig. 416. Telogen Effluvium
|
Marasmus:
is due to protein-calorie deficiency, usually in the first year of
life. The hair is fine and dry; the diameter of the hair bulbs is
reduced to a third of normal and almost all follicles are in
telogen state.
Kwashiorkor disease: occurs during the second year of life in children
suddenly weaned to a diet very low in protein and high in
carbohydrate. The hair changes are grossly similar to those in
marasmus, but there are more anagen follicles although most are
atrophic. In both states the hair is brittled, falls easily where partial or complete alopecia may occur. The hair is lusterless and
if normally black, may assume a reddish tinge. Many hair shafts
may show constrictions, which increase susceptibility to mild
trauma leading to hair shedding.
Iron
deficiency: is occasionally associated with diffuse alopecia,
even in the absence of anemia.
Zinc
deficiency: resulting from a failure in absorption gives rise
to alopecia and cutaneous changes as in acrodermatitis
enteropathica and prenatal zinc deficiency. Zinc deficiency may
present with erythema, scaling, bullae and hair loss.
Parental
iron deficiency may also cause deficiency of essential fatty
acids. This results in erythema, scaling of the scalp and eyebrows
and diffuse alopecia.
-
Metabolic
Alopecia
In
homocystinuria, which is an inborn error in the metabolic pathways
of methionin, the hair is sparse, fine and fair.
In
hereditary aciduria , which is a rare inborn error of pyrimidine
metabolism, characterized by retarded physical and mental
development, macrocytic anemia, the hair is fine, short and
sparse.
Histidine,
tyrosine and arginine errors of metabolism : The hair is dry,
lusterless, tightly curled hair.
-
Cicatricial alopecia
Infections
whether bacterial or fungal and certain skin diseases such as
discoid lupus and lichen planus may cause destruction to the hair
follicles.
|
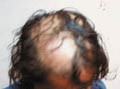
Fig. 417. Cicatrical Alopecia
|
-
Endocrinologic alopecia: occurs in the course of hypothyroidism and
hyper thyroidism.
-
Alopecia marginalis
usually
this type occurs in dark races where there is loss of hair from
the margins.


Fig.417b. Alopecia marginalis
Alopecia universalis
-
Trichotillomania
This type
is seen in neurotic children who pull the scalp hair and the
eyelids or eyebrows hair.

Fig.417b. Trichotellomania
-
Drug
induced alopecia
Different
types of drugs may induce hair loss . Methotrexate in cancer
therapy,Thallium, Colchicine, cytotoxic drugs, prolonged vitamin A
intake may cause alopecia.
Corticosteroids
may induce diffuse alopecia of the scalp together with lanugo hair
formation elsewhere.
Anti-coagulants
: heparin and coumarin may cause alopecia.
-
Hypervitaminosis
A
Excessive
consumption of vitamin A gives rises to a variable syndrome in
which the principal features are dryness, irritability and
sometimes pigmentation of the skin, and slowly progressive
thinning of scalp, body hair, eyebrows and eyelashes. Loss of
weight, fatigues, anemia and bone pain.
Liver and
spleen are sometimes enlarged.
-
Genetic
alopecia
This is an
autosomal dominant type of alopecia where racial factors play also
an important role.
-
Alopecia
areata with auto-immunity
Different
auto-immune diseases may be associated with alopecia mainly:
Alopecia is
associated with thyroid diseases.
The
association of vitiligo with alopecia
|
Pernicious
anemia.
Systemic
lupus erythematosus, rheumatoid arthritis, polymyalgia rheumatica,
myasthenia gravis, ulcerative colitis, lichen planus and the candida
- endocrinopathy syndrome .
|
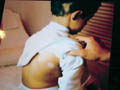
Fig. 418. Alopecia & Vitilligo (Autoimmunity) |
-
Pseudopelade
The term
pseudopelade is used to designate a slowly progressive cicatricial
alopecia, without clinically an evident folliculitis and no any
marked inflammation.
The
condition may occur in childhood . Pseudopelade is therefore
generally regarded as a clinical syndrome that may be the end
result of any one of a number of different pathological processes.
Lichen
planus and lupus erythematosus can produce a very similar clinical
lesion .
The
affected patches are smooth, soft and slightly depressed. At an
early stage in the development of any individual patch there may
be some erythema. The patches tend to be small and round or oval,
but irregular bald patches may be formed by confluence of many
lesions .The hair in uninvolved scalp is normal.
-
Alopecia
due to Physical Agents
Burns or
deep X-ray causes this type of alopecia .
-
Cosmetic
Alopecia
Chemicals
in cosmetic preparations as strong alkaline shampoos, different
topical applications of the scalp, hair gels and dyes.
Hydrogen
peroxide or other chemicals in hair dyes .
Excessive
use of hot combs or chessoirs.
Straightening
of hair.
-
Androgenic
Alopecia
Androgenetic alopecia (or male pattern baldness) begins with
recession of the frontal hairline. This is followed by thinning
over the vertex and then, eventually, complete loss of hair
over the crown. It is partially mediated by circulating
and locally produced androgens, including testosterone
and 5-dihydrotestosterone, combined with a genetic
susceptibility, possibly inherited in an autosomal
dominant fashion with variable penetrance.
Men who have been castrated before puberty and
homozygotes for 5 -reductase
type II deficiency do not develop androgenetic alopecia.
5 -reductase
type II deficiency do not develop androgenetic alopecia.
5 -Reductase is
the enzyme that converts testosterone to 5-dihydrotestosterone.
On the scalp of patients who are predisposed to the
condition, androgens lead to miniaturisation, a switch
from terminal to vellus or vellus-like follicles, and a
reduction in the duration of anagen. The concentration
of androgen receptor and 5 -Reductase is
the enzyme that converts testosterone to 5-dihydrotestosterone.
On the scalp of patients who are predisposed to the
condition, androgens lead to miniaturisation, a switch
from terminal to vellus or vellus-like follicles, and a
reduction in the duration of anagen. The concentration
of androgen receptor and 5 -reductase
activities in frontal hair follicles is greater than in
occipital follicles . Higher activities of aromatase, a
bifunctional enzyme involved in converting testosterone
to oestradiol, are found in occipital hair follicles.
This may explain the loss of hair in the frontal area
in androgenetic alopecia, while occipital hair is retained. In
women, in whom androgenetic alopecia expression is less severe
and often spares the frontal hair line, lower concentrations
of androgen receptors and 5 -reductase
activities in frontal hair follicles is greater than in
occipital follicles . Higher activities of aromatase, a
bifunctional enzyme involved in converting testosterone
to oestradiol, are found in occipital hair follicles.
This may explain the loss of hair in the frontal area
in androgenetic alopecia, while occipital hair is retained. In
women, in whom androgenetic alopecia expression is less severe
and often spares the frontal hair line, lower concentrations
of androgen receptors and 5 -reductase
activities are found in the frontal hair follicles, and
aromatase activities are higher. -reductase
activities are found in the frontal hair follicles, and
aromatase activities are higher.
Partial
baldness is sometimes first apparent on the vertex, but the most
frequent presentation of androgenic alopecia in women is a diffuse
hair loss.
Replacement
of terminal hairs by progressively finer hairs, which are
eventually short and virtually un pigmented.
Vellus
hairs are interspersed with hairs that are still normal and others
are only slightly reduced in diameter.
|
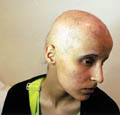
Fig. 419. Androgenic Alopecia (Alopecia & Acne)
|

Fig. 420. Same patiant After
treatment |
Treatment
of Androgenic Alopecia
Anti-androgens
The side
effects of anti-androgens preclude their use in men. In women,
there is some scientific evidence for regrowing of hair with
cyproterone acetate, but in general this drug, in doses of 50-100
mg/ day with ethinyl oestradiol, may be said to prevent further
progression of hair falling.
Finasteride is a 5 -reductase
inhibitor. Its use results in decreased circulating and scalp
concentrations of 5-dihydrotestosterone and a compensatory
rise in testosterone and gonadotrophin values. The androgen
receptor is not affected by finasteride Further hair
loss is prevented in most patients treated with finasteride. About
half of men achieve some regrowth, and in about a third, after
two years of continuous use, this is considered cosmetically important
To date, studies have examined the effect only at the
vertex, where the benefit is greatest. Less clinically dramatic
but statistically significant improvement in hair counts also
occur at the frontotemporal scalp margin, indicating that the
progression of hair loss in this region may at least be prevented.
Although regrowth may be seen as early as three months, patients
should be encouraged to take finasteride for two years before
evaluation. The prevention of further loss and the likelihood
of regrowth do not seem to correlate with the grade of
androgenetic alopecia. If treatment is successful it should
be continued indefinitely, as the balding process continues
when it is stopped. -reductase
inhibitor. Its use results in decreased circulating and scalp
concentrations of 5-dihydrotestosterone and a compensatory
rise in testosterone and gonadotrophin values. The androgen
receptor is not affected by finasteride Further hair
loss is prevented in most patients treated with finasteride. About
half of men achieve some regrowth, and in about a third, after
two years of continuous use, this is considered cosmetically important
To date, studies have examined the effect only at the
vertex, where the benefit is greatest. Less clinically dramatic
but statistically significant improvement in hair counts also
occur at the frontotemporal scalp margin, indicating that the
progression of hair loss in this region may at least be prevented.
Although regrowth may be seen as early as three months, patients
should be encouraged to take finasteride for two years before
evaluation. The prevention of further loss and the likelihood
of regrowth do not seem to correlate with the grade of
androgenetic alopecia. If treatment is successful it should
be continued indefinitely, as the balding process continues
when it is stopped.
The most common side effects, which occur in less than 2% of men,
are erectile dysfunction, diminished libido, and decreased ejaculate
volume. These effects are reversible and tend to be less of
a problem over time if the patient continues taking the drug.
To date, this agent has not be shown to be effective in
treating female androgenetic alopecia. (Recent
advances in dermatology).
Topical
preparations
Minoxidil
: Minoxidil 2%
-5% solution
(Regain) is a topical preparation used for treatment of hair fall
. It is a piperidinopyrimidine derivative and a potent vasodilator
that is effective orally for severe hypertension.
The
medication should be used twice daily for a long period not less
than 8 months.
When
applied topically containing 10% propylene glycol, Minoxidil has
shown conversion of vellus to terminal hair in up to 30% of
individuals.
-
Total
Alopecia
An
autosomal recessive gene usually determines total alopecia as an
apparently isolated defect. Many isolated cases may be associated
with other ectodermal dysplasia.
The scalp
hair is often normal at birth but is shed between the first and
sixth months, afterwhich, no further growth occurs.
|

Fig. 421. Congenital Alopecia |
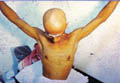
Fig. 422. Alopecia Totalis |
Alopecia
totalis
Loss of
the scalp and whole body hair . The problem may develop suddenly
or within few days or months .
|
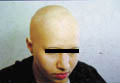
Fig. 423a. Alopecia Totalis
|
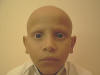
Fig. 423b. Alopecia Totalis |
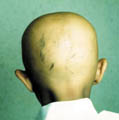
Fig. 424. Alopecia Totalis |
In some
cases the scalp has been totally hairless at birth where the child
lives with permanent alopecia .
Eyebrows,
eyelashes and body hair may also be absent.
Teeth and
nails are normal and general health, intelligence and expectation
of life are unimpaired.
-
Circumscribed
alopecia of congenital origin
Congenital
alopecia
This type is
usually associated with other ectodermal defects.
Clinical
Types
|
Naevoid
alopecia.
Epidermal
naevi are usually devoid of hair and present as warty or smooth but
slightly indurated plaques.
|

Fig. 425. Nevoid alopecia |
Aplasia:
of all layers of the skin gives rise to a congenital defect. There
is usually a circular or a linear area of scarring somewhat
depressed below the scalp surface commonly appears on the vertex.
Pseudopelade
may develop during
early infancy in association with certain hereditary syndromes, e.g.
incontinentia pigmenti and Conradi‘s syndrome.
Circumscribed
non-cicatricial alopecia:
is uncommon. It is the result of hypoplasia or aplasia of a group of
follicles. The scalp patches may develop between the third and sixth
months. This type may present with different types mainly :
Vertical
alopecia: a small
and often irregular patch of alopecia is present on the vertex at
birth.
Sutural
alopecia : multiple
patches overlie the cranial sutures.
Triangular
alopecia: a
triangular area overlying the fronto-temporal suture just inside the
anterior hairline, and with its base directed forwards.
Seborrheic
alopecia: occurs
with severe state of seborrhea where the hair loss may be localized
or diffuse.
Trichorerhexis
nodosa: this is britling of the hair due to follicular
dysfunction, which produces nodal swelling along the fibers leading
to hair fiber fracture and alopecia.
Menke‘s
kinky hair disease
The hair
becomes sparse, kinky and short due to fiber fracture.
Physical and
mental abnormalities where the condition may be fatal.
Diagnosis:
serum copper is decreased and copper accumulation in all body cells.
SYNDROMES
ASSOCIATED WITH ALOPECIA
-
Universal
alopecia
This
syndrome is characterized by:
Congenital
deafness
Spiny
hyperkeratosis
Universal
alopecia
Gastrointestinal
polyposis manifests with vomiting , diarrhea and abdominal pain .
-
Papillon-Lefevre
syndrome
Clinical
Features
Hyperkeratosis
of palms and soles
Hyperhidrosis
Alopecia
-
Cartilage
hair hypoplasia
Clinical
Manifestations
Abnormal
fine and sparse hair in children .
Limb
dwarfism
Recurrent
respiratory tract infection.
-
Marinesco-Sjogren
syndrome
Clinical
Manifestations
Congenital
cataract
Mental
retardation
Cerebellar
ataxia
Mental
retardation
Thin
brittled, sparse hair.
-
Hallman
-Streif syndrome
Clinical
Features
Hypotrichosis
Birdlike
faces
Microcephalus
Micrognathia
Congenital
cataract
-
Lipodematous
alopecia
Alopecia
Joint
hyperlaxity and hyperelasticity .
-
PROGERIA
Failure of
development normally after the first year of life .
Clinical
Features
Premature
senility .
Large bald
head and absent eyelids and eyelashes .
Skin :
wrinkled , pigmented and atrophied .
Subcutaneous
fat is decreased or absent .
-
Turner‘s
syndrome
Clinical
Features
Alopecia
of the frontal area of the scalp.
Low
hairline on the back.
Typical
webbing.
Short
stature.
Prominent
ears.
Increased
carrying angle.
Cubitus
vulgaris.
Cutix
laxa.
Webbing of
the neck.
Coaractation
of the aorta.
-
Noonan‘s
syndrome
The
clinical manifestations are the same as Turner‘s syndrome
without aortic coaractation.
-
Klippel-Feil
syndrome
Occurs
mainly in girls.
Clinical
Features
Low
posterior hairline.
Short neck .
Fused
cervical vertebrae.
Strabismus,
nystagmus .
Cleft
palate.
Bifed uvula.
-
Werner‘s
syndrome
Clinical
Manifestations
Alopecia.
Premature
hair graying.
Short
stature.
Atrophy of
muscles and subcutaneous tissue .
Spindle
extremities due to bone atrophy and osteoporosis .
Cataract.
Skin
changes : poikeloderma , diffuse hyperpigmentation with dark gray
and hyperkeratosis.
Hypogonadism.
-
Graham
-Little syndrome
Occurs
mostly after puberty and is characterized by:
Cicatricial
alopecia of the scalp.
Non
cicatricial alopecia of the axilla and pubic hair.
Lichen
planopiliaris.
Pseudopalade.
Treatment of
Alopecia Areata
General
Correction
of the predisposing factors such as anemia , emotional factors,
infections and others.
Usually the
condition is reversible. Hair may begin to regrow in the bald area
in a short or long time without treatment.
Topical
preparations
Many
preparations are used to treat alopecia, where some of these have an
effect sometimes, while others are used as a result of the advice of
non-professionals. In certain cases complications and waist of time
and money is the end result.
The simplest
method is to paint the area with an irritant such as tincture
iodine; Psoralenes lotion (Meladenin) that may cause irritation and
erythema due to increased vascularity of the area. After improvement
of irritation, hair may begin to grow. The traditional method of
treatment, which is usually free of charge is advised by barbers (
who by the way are usually the first to spot and diagnose alopecia)
is to scratch the area by his scalpel and rub it vigorously with one
or two lobes of garlic . In spite of the severe irritation, honestly
to say that we have been faced by a number of patients who are
satisfied with the results of treatment and they had their hair
grown again.
Different
local applications may be used containing Cantharides, capsicum
,tincture iodine, Gaborandi and others .
Minoxidil
preparations: These
may give good results if are used for a long time (6-8 months).
Corticosteroids:
These may give results, if used for a long time.
Topical
corticosteroids:
Local
infiltration by triamcinolone (Leddercort ) by syringe or dermojet.
Much care must be considered to use diluted steroid preparations in
order not to cause skin atrophy or hypopigmentation, which may
result from the concentrated corticosteroids during infiltration of
the area.
Systemic
medications are
rarely needed . Severe cases of alopecia my need prednisone tablets
or Depot medrol injections once weekly for 1-2 months.
|





















