|
The skin has very
important vital functions for keeping the physiological and biochemical
conditions of the body in its optimum state. The most important functions
of the skin are:
-
Regulates body
temperature.
-
Prevents loss of
essential body fluids, and penetration of toxic substances.
-
Protection of the
body from harmful effects of the sun and radiation.
-
Excretes toxic
substances with sweat.
-
Mechanical support.
-
Immunological
function mediated by Langerhans cells.
-
Sensory organ for
touch, heat, cold, socio-sexual and emotional sensations.
-
Vitamin D synthesis
from its precursors under the effect of sunlight and introversion of
steroids.
The epidermis is the
outer most layer of skin that acts as a barrier preventing toxic chemical
and other materials from penetrating deeper into the skin. This is
relatively porous and undergoes changes in thickness in response to
different factors such as trauma or pressure.
The layers of the
epidermis differentiate and gradually develop to a more rigid structure,
which provides a barrier to excessive loss of body fluids and the
penetration of noxious substances. The basal layer is the precursor of the
different cells of the epidermis which divide, pushed further upwards,
loosing much of their metabolic function and enzymatic activity. The
spinous layer is characterized by growth of keratin fibrils where these
are present also in the cells of the basal layer.
Epidermal cells as they
are pushed up away from the basal layer, begin to dehydrate and become
filled with cross-linked keratin, which gives the cells a granular
appearance. Lamellar bodies containing structured lipids play an important
role in skin protection. The intercellular lipids, the corneocytes, amino
acids, and other salts from sweat, sebaceous secretions, degradation
products from corneal proteins besides lipids and others all have an
important barrier effect preventing loss of water and keep the skin pH in
its optimum condition (5.5).
The stratum corneum
provides most of the barrier function.
The skin acts as a
two-way barrier to prevent the inward or outward passage of water and
electrolytes. The epidermis largely represents the barrier; whereas once
the epidermis is removed the residual dermis is almost completely
permeable.
There are two possible
routes for the passage of drugs through the epidermis, through the
transcellular, which is probably the major pathway for polar substances,
and through the intercellular.
|
FACTORS
AFFECTING SKIN PENETRATION
The penetration of substances through the skin surface depends upon
different factors:
|
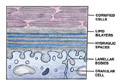
Fig. 8. Stratum corneum
with
the intercellular lipid layers
|
-
Age - penetration is
more in newborn and children than in adults.
-
Skin condition -
penetration is more on injured or abraded skin surfaces. Chemicals may
cause injury and increase penetration.
-
Hydration of the skin
- penetration is more in hydrated skin than dry skin. Hydration
increases the permeability of the stratum corneum. Water is an
effective penetration enhancer.
-
Fat content of the
epidermis has no much effect on penetration.
-
Type of vehicles:
vehicles may increase penetration and absorption of the drug from the
skin surface. This depends on the type of vehicle and the condition of
the skin. Certain vehicles that may cause injury to the skin even
minimal injury predispose to more penetration of the drugs or other
materials applied topically to the skin surface.
-
Hyperemia -
vasodilatation of the blood vessels in response to different stimuli
either local or generalized increases the penetration.
-
Physiological and
pharmacological factors
The penetration in vivo
of topically applied substances can be assessed by physiological or
pharmacological signs or analyzed by chemical or histological techniques:
-
Vasoconstriction has
been utilized for corticosteroids.
-
Vasodilatation for
nicotinates.
-
Whealing for
histamines.
-
Sweating for
pilocarpine.
-
Anesthesia for local
anesthetics.
-
Lipoid soluble
substances facilitate penetration of substances applied to the skin
surface. Steroid hormones and vitamin D, salts such as chloride and
sulfate can penetrate the skin surface. Gases and volatile substances
can pass through the skin.
REFERENCES
-
Abraham W, Downing
DT. Preparation of model membranes for skin permeability studies using
stratum corneum lipids. J Invest Dermatol 1989; 93: 809-13.
-
Breathnach AS.
Embryology of human skin. A review of ultrastructural studies. The
Herman Beerman Lecture. J Invest Dermatol 1971; 57: 133-43.
-
Breathnach AS. An
Atlas of the Ultrastructure of Human Skin. London: J. & A.
Churchill, 1971.
-
Biochemistry and
Physiology of the Skin Vol 2. New York and Oxford: Oxford University
Press, 1983: 1255-95.
-
Blank IH. Cutaneous
barriers. J Invest Dermatol 1965; 45: 249-56.
-
Elias PM. Epidermal
lipids, membranes, and keratinization. Int J Dermatol 1981; 20: 1-19.
-
Deutsch TA, Esterly
NB. Elastic fibers in fetal dermis. J Invest Dermatol 1975; 65: 320-3.
-
Farmer ER, Hood AF,
eds. Pathology of the Skin. London: Prentice Hall International, 1990.
-
Goldsmith LA, ed.
Biochemistry and Physiology of the Skin 2nd edn. New York: Oxford
University Press, 1991.
-
Holbrook KA, Odland
GF. Regional development of the epidermis in the first trimester
embryo and the second trimester fetus (ages related to the timing of
amniocentesis and fetal biopsy). J Invest Dermatol 1980; 74: 161-8.
-
Holbrook KA, Hoff MS.
Structure of the developing human embryo and fetal skin. Semin
Dermatol 1984; 3: 185-202.
-
Hashimoto K, Gross
BG, Lever WF. The ultrastructure of the skin of human embryos. I. The
intraepidermal eccrine sweat duct. J Invest Dermatol 1965; 45: 139-51.
-
Lever WF,
Schaumburg-Lever G. Histopathology of the Skin 7th edn.
-
Briggaman RA, Wheeler
CE. Epidermal-dermal interactions in adult human skin. II. The nature
of the dermal influence. J Invest Dermatol 1971; 56: 18-26.
-
Montagna W, Yun JS.
The skin of primates. XVI The skin of Lemur mongoz. Amer J Phys
Anthrop 1963; 21: 371-81. Philadelphia: Lippincott, 1990.
-
McKee PH. Pathology
of the Skin. Philadelphia: Lippincott, 1989.
-
Scheuplein RJ,
Bronaugh RL. Percutaneous absorption. In: Goldsmith LA, ed.
-
Smith JG, Jr, Fischer
RW, Blank H. The epidermal barrier: a comparison between scrotal and
abdominal skin. J Invest Dermatol 1961; 36: 337-41.
-
Scheuplein RJ,
Bronaugh RI. Percutaneous absorption. In: Goldsmith LA, ed.
Biochemistry and Physiology of the Skin Vol II. New York and Oxford:
Oxford University Press, 1983: 1255-95.
-
Wertz PW. Lipids of
keratinizing tissues. In: Bereiter-Hahn J, Matoltsy AG, Richards KS,
eds. Biology of the Integument. Vol 2: Vertebrates. Berlin: Springer-Verlag,
1986; 815-23.
-
Yardley HJ. Epidermal
lipids. In: Goldsmith LA, ed. Biochemistry and Physiology of the Skin.
New York: Oxford University Press, 1983: 363-81.
Top
|
