|
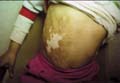
DISTURBANCE OF PIGMENTATION
|
|
|
|
Melanocyte activity has a more effect than the number of melanocyte density in the skin. The number of melanocytes in Negroes is not more than that available in the Caucasians.
Disturbance in skin color is either: Hyperpigmentation: which is mainly after, sunbathing, post inflammatory, hormonal or associated with different diseases. Hypopigmentation: follows certain skin diseases. Complete loss of pigment: such as in vitilligo and albinism. Skin color is due to melanin, which is synthesized by the melanocytes in the epidermis and hair follicles, from phenylallanin through transformation of tyrosine to dopa or dopamine and to dopaquine by the action of tyrosinase enzyme. In human beings there are three types of melanin: Eumelanin: insoluble brown pigment, which gives the skin its brown color, synthesized from phenylallanin. Phaeomelanin: gives the red hair synthesized from cystine and tyrosine. Neuromelanin: the pigment of substantia nigra. The color of the skin depends on other factors mainly:
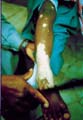
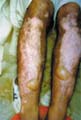
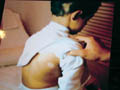
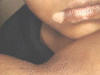
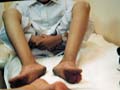
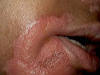
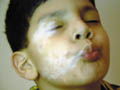
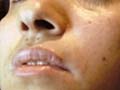
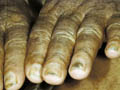
Vitilligo is a pigmentary skin disorder, characterized by sharply defined depigmented patches due to deficiency or destruction of melanocytes. Immunologic factors are considered in the etiology of vitilligo and there is herido-familial occurrence of the disease. Clinical Features The lesions appear usually on the exposed body surface such as the face and limbs. These are sharply demarcated milky white, depigmented patches, which may show hyperpigmented edges, especially with the progress of treatment. Vitilligo may be idiopathic or secondary to certain factors. Certain systemic diseases may be associated with vitilligo: thyrotoxicosis, anemia, gastric carcinoma, diabetes and Addison‘s disease. Course of Vitiligo The patches may repigment spontaneously or as a result of treatment, become stationary for a long period, or become very extensive covering the whole body with complete change of all skin surface color and hair. Treatment Different lines of treatment are used. Psoralenes and PUVA: are the mostly used since longtime till now, using trisoralen tablets and exposure to sun or PUVA after two hours from taking the medications. Common side effects may occur as photosensitivity or sometimes exacerbation of the lesions. Fig.318c. Photosensitization due to topical psoralene (Oxysoralene lotion) **Care should be considered especially when treating mucocutaneous areas Psoralenes are not indicated in children, where these age groups can be treated by topical 15-20 per cent oil of pergamount or Oxysorolene topical preparation and sun exposure before three o‘ clock in the after noon, preferred in the morning. Correction of any abnormality: such as anemia or associated diseases. Steroids topically or systemically: in form of long acting steroid such as (Depot medrol, 40 mgm) given weekly or oral Prednisolone tablets give good results in some cases. For young children we use the following methods of treatment: Topical 15 per cent oil pergamount twice daily in the morning, and topical mild steroid cream at night. In some cases, in older children we give Depot medrol 40mgm every two weeks for a total of four injections, for two months. We achieve good results, where repigmentation begins usually in the second week of treatment. We emphasize on the family of the child not to discontinue treatment, where we found that when repigmentation begins and stopping treatment, progressive repigmentation is very difficult. The patches seem to get resistance with little or no response to treatment. Micropigmentation and other camouflage locally: are used for patches of the face or fingers and areas, which sometimes resist treatment. Skin graft and melanocytes implantation are expensive and not always successful. I had in my mind an old experience concerning using plant photosensitizers for treatment of leucoderma and vitilligo. This was an important note I have to remember since a long time and to tell now after decades. I remember 50 years ago, when the natives of our village used to instruct patients having leucoderma or vitilligo to go to the farms in the morning and to injure the stem or remove the leaves of a fig tree, and apply the milky secretion on their skin lesions before exposure to sunlight. It is a primitive experience but it could do a lot for the patients who were satisfied with the erythema and regimentation of their lesions. Later, after a long time, I could find an explanation to that type of primitive natural dermatological practice. By experience, which may be inherited from grandfathers, they could find something to treat such skin problems in the time where there were no any alternative means. Narrow-band UVB Photography Narrow band laser
treatment for vitilligo and psoriasi has been considered recently as
an effective line of therapy for psoriasis especially cases which
don't respond to the traditional methods of treatment.Although this
type of treatment is expensive,yet it is the line of choice for
those who can afford paying for narrow band costs. Compared with broadband UVB, in the treatment of psoriasis, Narrow band UVB treatment has the following features: * Exposure times are shorter but of higher intensity. * The course of treatment is shorter * It is more likely to clear the psoriasis * Longer periods of remission occur before the psoriasis reappears For patients with psoriasis severe enough to require phototherapy, narrow-band UVB offers efficacy superior to conventional UVB and appears intrinsically safer than PUVA. However, because it produces more epidermal damage than wideband UVB, the narrowband treatment must be used with careful individualization of dosage and patient monitoring, according to James G. Krueger, MD, PhD.
Albinism is a partial or complete congenital absence of color of skin, hair and eyes due to decrease or absence of melanization. Albinism is usually associated with other defects and syndromes. Albinism is transmitted as a simple recessive trait, where there is a genetic absence of tyrosinase enzyme essential for oxidation of tyrosine to dihydroxyphenylalanin. Melanocytes are active, but melanin cannot deposit upon the premelanosomes. The defect is in the transfer of pigment to the keratinocytes in spite that tyrosinase activity is present. In such cases there is no tyrosinase activity and melanin synthesis, which ead to milky white dry skin, white hair, pink iris. Photophobia, skin atrophy and cancer due to loss of the protection ability of skin from the effect of sunlight. Albinism may be complete or partial, involving localized area of the skin surface. The manifestations appear at birth where, there is a localized depigmented patch that may have a progressive course to total depigmentation in older infants and children. The skin is paler instead of white, where islands of regimentation appear later on and the iris is light blue due to partial melanization. The hair is golden instead of white as in the complete albinism.
SYNDROMES ASSOCIATED WITH ALBINISM Piebaldism Genetic pigmentary disorders of melanocytes of skin and hair presenting with patchy depigmentation of the skin and a white forelock. Depigmented lesions may appear at birth, where the lesions remain unchanged throughout life. The disorder is transmitted as an autosomal dominant trait. The white forelock and the associated triangular patch of depigmentation on the forehead are diagnostic. Skin depigmentation is in the form of islands of residual pigmentation in the lesions and a line of pigmentation in the mid-line on the back and front of the legs, face and the back of the trunk. Metabolic disorders In phenylketonuria: there is pallor of the skin due to decrease of phenylanaline oxidase, which impairs hepatic formation of tyrosine from phenylalanin. Skin diseases Dermatoses causing inflammation resulting in destruction of the basal layer of the epidermis, such as discoid lupus erythematosus or in fungal infections of skin which act as melanocytes-destructive agents. Waardenburg‘s syndrome The manifestations of this syndrome are piebaldism, pallor of the iris, wide epicanthic folds and nerve deafness. Incontinentia pigmenti A genetic disorder almost in females characterized by skin manifestation appearing after birth, usually in the first, month in the form of small vesicles or blisters, nodules and later warty lesions followed by bizarre, linear or whorled pigmentation in the second year of life. Other manifestations of incontinentia pigmenti are absent teeth, epilepsy, mental retardation, spastic paresis, microcephaly, eye abnormalities such as nystagmus, pappilitis, choroidoretinits, alopecia and nail dystrophy.
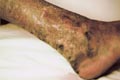
DIFFERENT
DISEASES AND SYNDROMES Different factors can produce local or generalized skin color changes and the differential diagnosis is often difficult. Urticaria pigmentosa Hypermelanosis is a characteristic feature of urticaria pigmentosa. In the childhood type: the light brown macules often exceed 2 cm in diameter and the lesions are frequently nodular. In the adult type: the smaller and more numerous macules are purplish brown in color and not palpably infiltrated, and often fail to urticate on friction. They are usually widely distributed over the trunk and limbs. Yellow pigmentation Jaundice is associated with hypermelanosis in biliary cirrhosis. Carotenaemia: Yellowish discoloration of the skin that is more common in children and vegetarians, where excessive carotene can be demonstrated in blood and urine. This may result from excess ingestion of certain foodstuffs rich in vit. A such as carrots, spinach, beans, yellow corn, sweet potato, and orange. Yellow coloration appears mainly on the palms, soles forehead and the nasolabial folds. Diabetes: The yellow coloration in diabetes may be due to hyperlipemia or dietary intake. Myxedema Chemicals: dinitrophenol, picric acid, trinitrotoluene, santonin, acriflavine, Mepacrine may cause hyperpigmentation. Hemosiderosis Dark red or red-brown, often with hypermelanosis of the lowers legs in stasis dermatitis, Sickle-cell anemia, congenital hemolytic anemia, Schamberg‘s disease and Majocchi‘s disease. Reactions to clothing Excessive excoriation and rubbing of the clothes against the skin causes localized hyperpigmentation corresponding to the affected areas. Metallic pigmentation Argyria: silver causes blue-gray hyperpigmentation, which is most intense on exposed areas of skin. Bismuth: causes blue-gray hyperpigmentation resembles argyria but bismuth line on gums is more common than skin pigmentation. Mercury hyper-pigmentation: causes gray-brown discoloration of the skin, which is limited to sites of repeated application of mercurial ointments - especially on the eyelids and skin creases Cosmetics: The skin pigmentation depends on the type of topical preparation.
Lentigo is hyperpigmented, benign, discrete macules that occur mostly on the sun exposed areas due to increased activity of epidermal melanocytes. The lesions may be multiple, appearing in early life and continue till puberty mainly on the upper part of the body and may be associated with pulmonary and aortic stenosis, skeletal abnormalities and genitalia defects. Differential Diagnosis Junction nevus. Pigmented seborrheic keratoses. Treatment Q-switched ruby laser is recently used as an effective device to clear lentigo. C02 Laser can also give good results for ablation and resurfacing of lesions. Liquid phenol neutralized with alcohol is an old treatment. Topical bleaching creams such as 4% Eldoquine may give some effect. Drug induced hyperpigmentation Chloropromazine, Busulphan, Inorganic arsenic, and ACTH causes generalized pigmentation and remains unchanged through out life, where there is patchy depigmentation of the skin and white forelock with diagnostic triangular patch of depigmentation on the forehead. Pigmentation may be induced by a wide variety of other drugs. Several mechanisms are involved in the drug-induced changes of pigmentation of the skin. Certain heavy metals may be deposited in the dermis in sufficient quantity to bring about a distinctive change in skin color without any significant increase in melanin. Fixed drug eruptions hyperpigmentation occurs due to damage of cells in the basal layer such as with Sulfonamides. The ‘gray baby‘ syndrome is due to chloramphenicol overdose. Topical photosensitizers may cause localized skin hyperpigmentation.
This is a rare inherited disease, affecting children, characterized by generalized dusky or olive-brown pigmentation, congenital defects and usually accompanied by hematological abnormalities. Clinical Features The commonest sites involved are lower trunk, flexures and the neck. Skin manifestations Generalized dusky hypermelanosis, appear with scattered over the dusky areas, depigmented macules of raindrop type and macules of darker pigmentation. Rarely, only café-au-lait macules are present. General manifestation Affected children are mentally retarded, slender built with short, broad hands with tapering fingers and thumbs which are rudimentary. Microcephaly and hypogonadism are frequent besides other developmental defects. Hematological abnormalities Hematological changes are hypoplastic anemia, thrombocytopenia, neutropenia and fatal pancytopenia with hemorrhages are usually fatal in infants and young children. There is an increased incidence of acute leukemia and other neoplasms.
Etiology The cause of this syndrome is unknown. The full syndrome with precocious puberty occurs only in girls. Clinical Features Skin manifestations Cutaneous pigmentation usually develops between the ages of 4 months and 2 years, but may be present at birth. Extensive light-brown patches, often with an irregular or serrated margin, occur mainly on the trunk, buttocks and thighs, but may rarely involve the face and neck. They tend to be asymmetrical and to be most extensive on the sides. Bone manifestations Bone changes are severe such as aching pain, pathological fractures and secondary deformities. Eye manifestations Proptosis and defective vision are due to overgrowth of bone at the base of the skull. Hematological Findings. Serum calcium and phosphorus are normal, but alkaline phosphatase may be elevated if the bone lesions are numerous. General manifestations In females, precocious puberty, breast enlargement, vaginal bleeding and growth of pubic hair, occur below the age of 5 in about 50% of cases and between 5 and 10 in 30%. Growth in childhood is accelerated but the epiphyses unite prematurely. Other developmental abnormalities may be associated with the syndrome. The prognosis for life is good and the pathological fractures unite normally. Diagnosis There is no single clinical feature of the pigmented lesions which reliably differentiates Albright‘s syndrome from neuro fibromatosis in which bone lesions and endocrine disturbances may also occur. The presence of many cafe-au-lait macules freckles in the axillae and Lisch nodules on the iris are diagnostic for neuro fibromatosis. Giant pigmented granules may also rarely be found in Albright‘s syndrome.
This type can be considered as photodermatitis. Clinical Manifestations. Skin lesions appear as an erythematous, pruritic pigmentation, which is more intense on the sun-exposed areas, mainly on the forehead, neck, behind the ears and areas of friction such as the axilla. The characteristic features are spotty pigmentation, light to dark brown in color. Hyperkeratosis, hyperemia and telengectasia may be other manifestations. This type should be differentiated from berloque dermatitis, which is hyperpigmentation due to photosensitization, by certain types of perfumes.
NAEGELI-FRANCESCETTI-JADASSOHN SYNDROME This rare syndrome is inherited as an autosomal dominant, that affects young children. Clinical Manifestations Skin manifestations Hypermelanosis is of the reticulate type of pigmentation that develops on the neck and axillae during the second or third year in a previously normal child. It may become very extensive and is not preceded by any inflammation. Keratoderma of the palms and soles is usual. General manifestations Hypohidrosis with intolerance to heat is common. Hair and nails are normal. Teeth may be normal or defective, with yellow discoloration of the enema. Mental and physical development is normal.
This syndrome is inherited as a sex-linked that affects young children between 5 and 13 years of age. Clinical Manifestations Skin manifestations Skin has a poikilodermatous appearance with atrophy and prominent telangiectasia. Reticulate hyperpigmentation is most conspicuous on the neck, chest and thighs. Mucous membranes: leucoplakia of the oral, ocular and anal mucous membranes. General manifestations Nail dystrophy. Hematological abnormalities are common.
This syndrome begins in early life. This is different from Becker‘s nevus. Clinical manifestations Discrete or confluent brown macules appear on the neck and forearms. Hyperpigmented areas may develop later. Small white macules appear in the pigmented areas. Diffuse pigmentation with conspicuous macular depigmentation appears on the trunk, associated with macular and reticulate pigmentation of the neck.
HERIDETARY
UNIVERSAL MELANOSIS Pigmentation is usually present from early infancy but it may be progressive. It is often diffuse and generalized but may later become rather mottled.
“Café-au-lait“ macules and plaques are present in 90% of cases of neuro fibromatosis and may appear early. They are round or oval patches of light brown pigmentation. The presence of one or two macules is not diagnostic in the absence of other signs of the disease, but if six or more are present the probability of neuro fibromatosis is high. Extensive melanotic macules can also occur and resemble those seen in Albright‘s syndrome; however, these tend to be confined to a particular site and are on either side of the mid-line. Axillary freckling is common in neuro fibromatosis and is an aid to the diagnosis. Lisch nodules and iris hamartomas are present in most patients over the age of 6.
Clinical Feature In the acute infantile form of Gaucher‘s disease, the skin is not pigmented but in Niemann-Pick disease, there is diffuse brown pigmentation, most marked on the face. Pigmentation of two types occurs in adults with Gaucher‘s disease. Brown patches of cloasma type appear on the face, neck and hands.There are symmetrical pigmentation of the lower legs with a sharp lower margin and an irregular upper margin. There may be a brown wedge-shaped thickening of the bulbar conjunctiva.
Xeroderma pigmentosum (XP) is a rare autosomal recessive disease characterized by photosensitivity, pigmentary changes, premature skin aging, neoplasia and abnormal DNA repair. Some patients with xeroderma pigmentosum have, in addition, neurological complications. Oral retinoids can reduce the occurrence of skin cancer in XP.
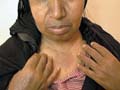
Addison‘s disease is characterized by diffuse pigmentation on the sun exposed areas, flexures, sites of pressure or friction and mucous membranes due to increased secretion of melanotrophic hormones by the pituitary and elevated plasma levels of beta-MSH-. Nipples, genitalia, buccal mucosa and conjuctiva become deeply pigmented. Vitiligo-like lesions may also occur in Addison‘s disease. Pigmentation of Addisonian pattern has been noted in 10% of reported patients with Cushing‘s syndrome. It is an indication of increased secretion of ACTH and beta-MSH by the pituitary, which may be due to a pituitary tumor. After adrenalectomy a progressive hypermelanosis may develop in spite of adequate hormone replacement therapy. Only in half of these patients, the sella turcica is enlarged. These patients show marked hypermelanosis of the skin and mucous membranes. Clinical Manifestations Hypermelanosis of the skin and mucous membranes. The hair is often darker. Nails show sometimes multiple lentigines and longitudinal pigmented bands. Very high levels of both beta-MSH and ACTH are found in the plasma.
|
| Contents | << Previous Chapter | Next Chapter >> | Search |