|
DERMATOSES DUE TO PHYSICAL INJURIES
|
|
|
|
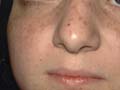
Actinic injury: The different clinical manifestations of actinic injury are: Photo-allergic dermatitis Photo-toxic dermatitis Chronic actinic dermatitis Sunburn Polymorphous light eruption Freckles Xeroderma pigmentosum Colloid milium Hydroa vacciniforme Radio dermatitis Neonatal cold injury Skin tumors mainly melanomas.
The incidence of sunlight that can induce skin tanning and photo damage has been increased in the past few years. Children and susceptible individuals especially those with light colored complexion of the skin are more susceptible to the harmful effect of sun. Serious and even fatal problems due to melanoma and non-melanoma skin cancer do occur due to unwise excess exposure to sunlight. That is “a hazardous effort for a trivial cosmetic bronzing reward“.
The radiation striking the earth is either visible or invisible light. The harmful effect of the light spectrum is the UV radiation. Ultra violet is of two types; UVA (10 per cent), where it‘s intensity declines from the noontime and UVB which constitutes (90 per cent) of the UV reaching the ground. Solar radiation includes the electromagnetic spectrum, which begins from the short, high energy cosmic, gamma and x-ray to the longer energy ultraviolet (UV), visible, infrared (IR), microwave and radio waves. Most of the harmful solar radiation is absorbed high in the atmosphere by the ozone at around 20 kilometers above the sea level. Factors affecting skin reaction Skin reaction due to the effect of sunlight depends on different factors mainly:
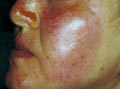
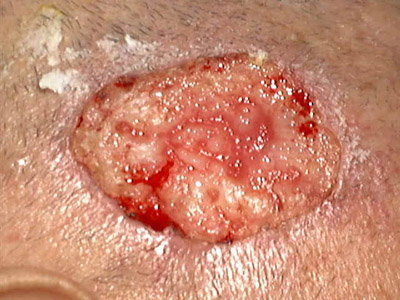
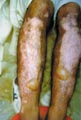
Immunologic factors Immunologic factors have an important role. Patients who have photosensitivity will have a direct effect on the sun-exposed areas and may involve also covered areas of the body. Drugs Systemic drugs: The effect of solar radiation is more severe with patients who are receiving medications causing photosensitization such as Tetracycline or Phenothiazines. Topical preparations: Topical Psoralenes, plants containing Furocoumarines, perfumes and cosmetic preparations may act as photosensitizers causing photodermatitis. Clinical manifestation of effect of sunlight. A. Acute solar reaction. Sunburn Erythema is the immediate response that may be mild or severe. Vesiculo bullous eruption appears later on the exposed areas with severe burning sensation and oozing of the skin surface. The reaction may be a burn of the first or second degree. The severity of erythema depends on different factors mainly the skin color where it is more in blond and white races. Melanin in the dark skinned individuals acts as a protective screen from the effect of sunlight, where it reflects, absorbs and scatters ultraviolet radiation. The type of reaction due to sun exposure is an immediate erythema, photodermatitis or sunburn due to UVA or delayed erythema, which begins after few hours from exposure to UVB radiation. UVB has an effect on the exposed and covered parts of the body on contrast to UVA that has its effect on the sun exposed areas. This reaction may resolves after few days leaving skin tanning. Tanning occurs as a result of increased production of melanin in the melanocytes in response to UVB, which increases the binding of the circulating melanocyte stimulating hormone to the melanocytes leading to melanocyte proliferation, Dendritic arborization leading to skin tanning. B. Photo toxic reaction C. Photo allergic reaction D. Polymorphous light eruption E. Chronic effect of sun exposure Chronic solar effect Skin tanning and thickening of the stratum corneum are the mildest hazard from chronic exposure to sunlight. Solar keratoses, melanomas and skin squamous carcinoma are very serious complication where fatal cases from melanomas are much increased during the past few years due to excess sun exposure especially on the sea shores to get tanned skin. Wrinkles and premature skin aging due to collagen degeneration from the effect of sun light. Photodynamic and phototoxic reactions. Drugs and other chemicals with photodynamic and phototoxic activity potentiate the pigmentogenic effect of UV lights causing photodermatitis. Tanning follows the sunburn-like reactions to certain drugs such as that of tetracycline, but not photoallergic reactions. If the photodynamic agent is applied directly to the skin the intensity of the pigmentary response is greatly enhanced and the hypermelanosis may be heavy and persistent. Phytophotodermatitis Phytophotodermatitis is an inflammatory and pigmentary reaction of the skin due to the effect of sunlight, predisposed by contact with furocoumarins in plants or other compounds. The reaction occurs in the areas exposed to sunlight after these plants have been crushed on the skin surface. There is some individual variation in susceptibility, but with adequate exposure most will react. If the inflammatory phase is severe, bullae are formed, but in milder cases only the pigmentary changes are conspicuous and follow the irregular pattern of the points of contact of the plant stems and leaves with the uncovered skin. The most common clinical syndrome is therefore a bizarre network of pigmented streaks, often on the legs and frequently in a child.
Berloque dermatitis results from the potentiation of the stimulation of melanogenesis by light by 5-methoxypsoralen or bergamot oil contained in perfumes, notably eau-de-Cologne.
The pigmentation occurs in susceptible subjects who have been exposed to light after the application of perfume. The distribution of the lesions is therefore variable but their configuration is usually distinctive. Deep-brown pigmentation follows the pattern formed by the droplets of perfume over the skin from their points of application. The pigmentation fades after weeks or months. The condition is now much less frequent, though it is a continuing cosmetic problem.
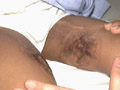
The hazardous effect of sun light exposure is more serious in infants and young age groups. Recorded deaths have been reported in several affected neonates, either from kernicterus or from extra hepatic biliary duct atresia. Phototherapy Phototherapy with blue light at 420-460 nm leads to the trans cutaneous photo-oxidation of bilirubin, and has become firmly established as a safe and effective treatment for neonatal. A number of minor cutaneous side effects have had been described. Some babies develop a macular erythematous rash. Darkening of treated areas of skin lasting for several months has been reported in racially black babies. “Bronze baby“ syndrome This is a rare complication of neonatal phototherapy in which a dark brown (‘bronze‘) pigmentation of the skin, serum and urine follows phototherapy, and remains as the hyper bilirubinaemia fades. Hepatic disease appears to be a prerequisite for the development of this complication. The bronze pigmentation gradually fades after discontinuation of phototherapy, but death has been reported in several affected neonates, either from kernicterus or from extra hepatic biliary duct atresia.
METHODS OF PROTECTION FROM THE EFFECT OF SUN The harmful effects of sun are strongest between 10 a.m. and 4 p.m.
Sunscreens are UV-absorber that contain certain ingredients such as p-amino benzoic acid esters, methyl-, phenyl- and benzyl salicylates, benzyl cinnamate, digalloyl trioleate (photosensitizer), 4-isopropyl-dibenzoylmethane, 3-(4-methylbenzylidene)-camphor and 4-tertiarybutyl-4'-methoxy-dibenzoylmethane. Sunscreens were presented in the market in 1928 as an emulsion of benzyl salicylic acid and benzyl cinnamate and later other sunscreens were available as quinine bisulfate and quinine oleate. Sun block usually reflects or scatters all UV rays. This should be applied about 20 minutes before exposure to sun and should be reapplied after two hours. It should be noted that children and other sensitive groups should be instructed to use sunscreens routinely, like brushing their teeth. Sunscreens of at least 15 SPF lip preparation is available and should be used to protect the lips from actinic injury. Eye protection from the effect of UV by using special sunglasses, which have the ability to block UVA and UVB wide brim hats can also have some protection. All skin types of different age groups especially infants and children need protection from solar UV. Those with Type I and Type II with blond and light skin color are more susceptible. Broad-spectrum sunscreens with an SPF of at least 15 offer substantial protection against sun burning, especially for fair-skinned people. It is very important to minimize exposure from 10 AM to 4 PM and try to be in the shade. Shade can‘t give complete protection from the effect of sun, since sand, water, snow and grass reflect UV rays even if the body is in a shady area. Umbrella used outdoors, on the seashores or personal one can give some protection . The most effective protection in all cases is the broad-spectrum sun block. Para-amino benzoic acid and its derivative is a popular sunscreen agent. Sunscreens containing p-amino benzoic acid esters, methyl-, phenyl- and benzyl salicylates, benzyl cinnamate, digalloyl trioleate, (photosensitizer) are used as sunscreens. It should be noted that some sunscreens may cause photosensitization. It is important to select the effective and non-sensitizing type of sunscreen.
Topical Sunscreen agents
(WEB MED) N.B. : More details can be found in chapter 05 " Dermatological treatment" PrecautionsAllergic reaction : sensitization to the active ingredient or the base of the sunscreen product may occur especially in patients having a history of an allergic reaction to drugs such as” caine” group such as benzocaine, anesthetics artificial sweetening agent such as saccharine, antidiabetics, analine dyes, sulfa , diuretics such as thiazides, perfumes , tooth paste, preservatives and others.-- .
Before every exposure to the sun, apply an appropriate sunscreen product that protects you against ultraviolet sun rays. For maximum sun protection, sunscreens should be applied uniformly and thickly to all exposed skin surfaces (including the lips, using lip sunscreen or lip balm). Sunscreen products containing aminobenzoic acid, lisadimate, padimate O, or roxadimate should be applied 1 to 2 hours before sun exposure. Other sunscreen products should be applied 30 minutes before sun exposure, unless otherwise directed by the package instructions. Lip sunscreens should be applied 45 to 60 minutes before sun exposure. Because most sunscreens are easily removed from the skin, you should reapply these products liberally every 1 to 2 hours for adequate protection. You should reapply sunscreen especially after swimming or heavy perspiration. Lip sunscreens should be reapplied liberally at least once every hour while you are in the sun and also before and after swimming, after eating and drinking, and during other activities that remove it from the lips.
Some sunscreen agents contain alcohol and are flammable. Do not use near heat, near open flame, or while smoking .
( webmed)
|
| Contents | << Previous Chapter | Next Chapter >> | Search |